Urodynamic Assessment: Voiding Studies
WHEC Practice Bulletin and Clinical Management Guidelines for healthcare providers. Educational grant provided by Women's Health and Education Center (WHEC).
Urodynamic tests are valuable for the assessment of voiding function. Numerous techniques have been developed to evaluate the types and extent of urinary incontinence. A number of treatment options exist, including behavioral, medical, and surgical approaches. Urinary incontinence affects 10-70% of women living in a community setting and up to 50% of nursing home residents. Prevalence of incontinence appears to increase gradually during young adult life, has a broad peak around middle age, and then steadily increases in the elderly. Most women with incontinence do not seek medical help. The estimated annual direct cost of urinary incontinence in women in the United States is $ 12.43 billion. The relative likelihood of each condition causing incontinence varies with the age and health of the individual. Among ambulatory women with incontinence, the most common condition is urodynamic stress incontinence, which represents 29-75% of cases. Detrusor overactivity accounts for 7-33% of incontinence cases, with the remainder being mixed forms. Among older, non-institutionalized women with incontinence evaluated in referral centers, stress incontinence is found less often, and detrusor abnormalities and mixed disorders are more common than in younger ambulatory women. More severe and troublesome incontinence probably occurs with increasing age, especially age older than 70 years.
The purpose of this document is to consider the best available evidence for evaluating voiding studies. Uroflowmetry is an electronic measure of urine flow rate and pattern. Combined with assessment of postvoid residual urine volume (PVR), it is a screening test for voiding dysfunction. If the uroflowmetry and postvoid residual volume (PVR) are normal, voiding function is probably normal; however, if the uroflowmetry or postvoid residual volume (PVR) or both are abnormal, further testing is necessary to determine the cause. More sophisticated measures of voiding function include a pressure-flow voiding study with or without videofluoroscopy. Electromyography of the striated urethral sphincter may be useful to assess neurogenic voiding dysfunction.
Uroflowmetry:
Uroflowmetry represents the interaction of detrusor contractility and outlet resistance. In the majority of patients with bladder outlet obstruction, increased outlet resistance results in a diminished urinary flow rate. Combined with a post void residual (PVR) measurement, it provides information on voiding flow rate, flow pattern, ability to empty and capacity. Uroflowmetry, or the measure of urine volume voided over time, is a simple and non-invasive test. It is performed by asking the patient to void in a special commode. Urine is funneled into a flowmeter that records volume versus time. It is important to get a representative flow pattern; this pattern depends on a number of factors. First, the patient should understand the simple nature of the test and be as relaxed as possible to have a normal desire to void at the time of the study. Second, the patient should be allowed to void in private because tension and embarrassment can artificially reduce the maximum flow achieved. Third, if there is doubt about the accuracy of the test, it is important to ask the patient whether he or she felt it was representative. If the patient believes that the test was not typical, it should be repeated. Even though uroflowmetry is not specific in identifying outlet obstruction, the flow rate remains an extremely sensitive indicator of lower urinary tract dysfunction.
Uroflow Meter: Various urodynamic techniques have been devised to study voiding. Commonly used flow meters use either weight, an electronic dip-stick, or a rotating disc to determine urinary flow rate. Modern electronic uroflowmeters are designed to provide high sensitivity and reproducibility data. The technical attributes that provide high sensitivity to a uroflowmeter is the time constant parameter. From a practical viewpoint, a time constant of 0.25 seconds mean that the flowmeter will register any change in the flow rate of at least 0.25 seconds duration. In the case of the maximum urinary flow rate, however, such high sensitivity may not be desirable, since it allows the flowmeter to capture even a brief artifactual change in the flow rate. This can occur by variation of the direction of the urinary stream during voiding and may be especially prominent when the stream strikes the rotating disc of the flowmeter, or with abrupt movement of either the weight or electronic dip-stick uroflowmeters.
Terminology:
Urinary flow is described not only by its rate, but also by its pattern, which may be either continuous or intermittent. The flow rate is defined as the volume of fluid expelled via the urethra per unit time, expressed in ml/sec. A properly performed uroflow rate determination should specify:
- Voided volume -- the total volume of urine expelled from the bladder.
- Postvoid residual urine (PVR) volume -- the total volume of urine remaining in the bladder after voiding.
- Patient environment and position -- supine, seated, or standing
- Filling -- by diuresis (spontaneous or forced) or by catheter (transurethral or suprapubic)
- Type of fluid voided
- Type of measuring equipment
- Solitary procedure or combined with other measurements
- An annotation specifying whether the recorded uroflow is typical of the patient's usual micturition pattern.
Definitions and Normal Parameters: Some basic concepts bear definition before further discussion of different types of flow rates and patterns are described below:
- Flow time (Qtime) -- the time over which measurable flow actually occurs
- Flow rate (Q) -- it is defined as the volume of fluid expelled via the urethra per unit time and is expressed in milliliters per second (ml/sec)
- Maximum flow rate (Qmax) -- the maximum measured value of the flow rate
- Average flow rate (Qave) -- it is voided volume divided by flow time. The average flow rate is only interpretable of flow is continuous and without aberrancy, either at the initiation or termination of voiding.
- Time to maximum flow -- the elapsed time from the onset of flow to the point of maximum flow
- Continuous urinary flow -- a constant urinary stream without interruption
- Mean flow rate (Qmean) -- volume voided divided by flow time
- Flow pattern -- subjective description of the regularity of voiding. The flow pattern must be described when the flow time and average flow rate are measured
- Intermittent flow -- flow pattern in which interruptions of varying duration occur between episodes of voiding. The same parameters used to characterize continuous flow may be used to describe intermittent flow only if caution is exercised. To quantify flow time, however, the time intervals between flow episodes should be disregarded. Conversely, the voiding time refers to the total duration of micturition, including the intervals between flow episodes. Therefore, if voiding occurs without interruption, voiding time is equal to flow time.
Among the many parameters provided by uroflowmetry, the maximum urinary flow rate (Qmax) is regarded by most experts as most useful not only in assessing the degree of bladder outlet obstruction, but also in monitoring treatment effects. Many attempts have been made to correct the maximum flow rate for age, sex, and voided or total bladder volume. It is currently assumed that correction or adjustment of the maximum flow rate value is unnecessary if voided volume exceeds 150 ml. The mean maximum flow rate in asymptomatic women is considered to be 26 ± 14 ml/sec, with an average voided volume of 224 ml. A normal peak flow rate for women is 20-30 ml/sec. A PVR of 25% or less of voided volume is acceptable.
Pattern: A normal flow pattern is represented by a bell shaped curve. Age-matched comparisons reveal that women generally display a higher mean and maximum flow rate than men, voiding similar volumes. However, the uroflow curve is rarely completely without variations. Fluctuation in the smooth voiding curve pattern is usually attributable to the effects of abdominal pressure or sphincteric activity.
Normal Uroflow Study Measurements:
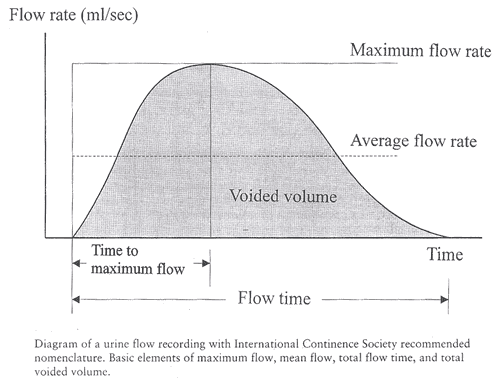
Uroflow study interpretation: An abnormally long, flat plateau with low average and maximum flow rates generally indicates outlet obstruction or decreased detrusor contractility. Intermittent flow has a saw-tooth appearance and can be secondary to abnormal straining or detrusor sphincter dyssynergia (where the striated urethral sphincter contracts simultaneously with the detrusor during voiding). Conversely, high flow rates may reflect decreased outlet resistance and/or increased abdominal effort. It is not possible to make these distinctions by uroflow. However, if impaired detrusor contractility would alter clinical management, then an abnormal uroflow may warrant further investigation. A patient who voids very quickly can produce what has been called a superflow pattern in which there is very little outlet resistance. This pattern can be seen in patients with severe stress incontinence. Abnormal uroflometric parameters can occur secondary to factors that affect detrusor contractility, urethral resistance, or both. Detrusor contractility can be affected by neuropathic lesions, pharmacologic manipulation, intrinsic detrusor muscle or bladder wall dysfunction, or psychogenic inhibition. Urethral resistance can be altered by tissue trophic changes producing atrophy or fibrosis, drug effects such as alpha-adrenergic stimulators, neuropathic striated muscle contraction, pain or fear, and urethral axis distortion secondary to severe pelvic relaxation. Outlet obstruction secondary to an intraurethral lesion or stricture is exceedingly rare in women. Extraurethral lesions, such as vaginal masses or cysts, and large enterocele or rectocele may compress the urethra, resulting in obstructed voiding. Detrusor-external sphincter dyssynergia is a condition between the detrusor muscle and the external striated sphincter. This leads to obstructed voiding and is always secondary to a neurologic lesion, most classically high spinal cord trauma.
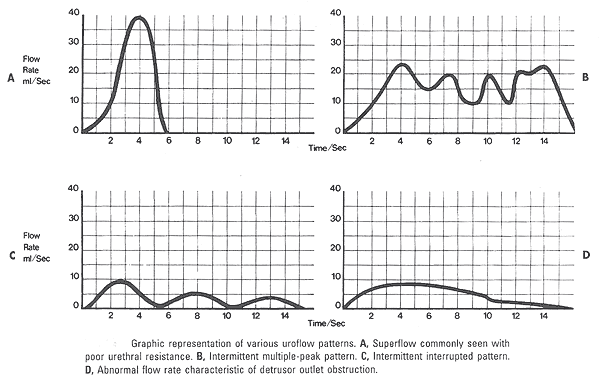
Clinical Applicability:
Some clinical situations in which spontaneous uroflowmetry may be useful are briefly discussed here. Symptoms suggestive of voiding dysfunction -- if uroflow measures are normal in patients complaining of symptoms consistent with voiding difficulty, further investigation is unnecessary. Abnormal flow rates would require further urodynamic testing. Frequency and urgency syndromes -- it is often necessary to find the urodynamic abnormality responsible for the symptom complex of frequency, nocturia, urgency, and urge incontinence. Flow studies are only preliminary to cystometry in this situation. Flow studies can also be used to evaluate treatment response. Before pelvic surgery -- women undergoing pelvic surgery, particularly suprapubic procedures for incontinence and radical pelvic surgery, and those who are elderly, have neurologic disease, or have had past pelvic surgery should have uroflowmetry performed. Neurologic disease -- when neurologic disease affects the lower urinary tract, various degrees of voiding dysfunction can result. Uroflowmetry is preliminary to more detailed urodynamic tests and at times can be helpful in the diagnosis, management, and prognosis of these patients.
Pitfalls: Bladder overdistention may be responsible for artifacts during uroflowmetry. Temporary impairment of detrusor contractility may be caused by overstretching of the detrusor muscle fibers. A second pitfall during uroflow evaluation is that of measuring only one flow parameter, such as peak flow. This may be misleading, because some patients may generate very high peak flows with straining maneuvers. Thirdly, in comparing flow rates in a given individual from one time to another, either for the purpose of evaluating treatment or following a given condition, it is important to standardize the rates to a given volume.
Pressure-Flow Studies:
A patient who presents with an abnormal uroflow or high PVR may be a candidate for further investigation. Most specialists agree that patients with normal uroflow results do not require pressure flow studies. It provides a detailed assessment of voiding through simultaneous recording of bladder, abdominal and true detrusor pressures along with uroflow data during bladder emptying. Pressure flow studies present the relationship between the detrusor and outflow resistance by measuring the contractility of the detrusor muscle, coordination between urethral striated muscle (relaxation) and detrusor smooth muscle (contraction), and the ability to empty completely. A pressure flow study can diagnose voiding dysfunction such as obstruction, detrusor sphincter dyssynergia or a weak, non-contractile bladder. To interpret a pressure flow study, first compare the study flow rate and pattern to the patient's noninvasive uroflow performed previously. If the voiding patterns do not look comparable, consider other factors such as patient inhibition or different voided volumes. The pressure flow study should confirm and further illuminate abnormal uroflow results. Second, evaluate the detrusor contraction strength. Note the numeric value for the maximum detrusor contraction, the relationship of the maximum flow rate and corresponding detrusor contraction strength, and the overall shape, pattern and quality of detrusor contraction.
Definitions: The following are definitions of standardized terminology proposed by the International Continence Society (ICS):
- Premicturition pressure -- it is the intravesical pressure recorded immediately before the initial isovolumetric contraction. It should be the same as the resting pressure at maximum cystometric capacity.
- Opening pressure -- it is the pressure recorded at the onset of measured flow. There is a delay of approximately 0.5 to 1 second in the recording of flow because of the time taken for urine to reach the flowmeter.
- Opening time -- it is the time elapsed from the initial rise in detrusor pressure to the onset of flow. This is the initial isovolumetric contraction period of micturition.
- Maximum voiding pressure -- it is the maximum value of the measured pressure during voiding.
- Pressure at maximum flow -- it is the pressure recorded at the time of maximum flow. Any delay in the recording of flow rate must be allowed for.
- Contraction pressure at maximum flow -- it is the difference between the pressure at maximum flow and the premicturition pressure.
- After-contraction -- describes the common findings of a pressure increase after flow cases. The etiology and significance of this event are unknown.
Methodology: These studies are usually performed after a cystometric evaluation and involve the monitoring of abdominal, intravesical, and true detrusor pressure synchronously with flow. External sphincter electromyographic (EMG) activity, as well as urethral pressure, also may be measured. To ensure that proper pressure transmission is occurring, the patient should be asked to cough before being allowed to void. With the patient in a sitting position, she is then instructed to void to completion if possible. It is very important during the voiding phase to respect the patient's privacy. Once flow is initiated, the patient can be asked to interrupt the stream suddenly (stop test). This test attempts to establish voluntary control of micturition and also obtains isometric detrusor pressure.
Interpretation: Normal pressure flow results for women include a detrusor pressure of 10-30 cm H2O, with an average flow rate of >20 ml/sec. Outflow obstruction is indicated by a maximum flow rate <15 ml/sec with a maximum detrusor pressure >50 cm H2O. Patient age and voided volume will affect normal values. Flow patterns in pressure flow studies are the same as for uroflowmetry. It is sometimes difficult to ascertain whether abdominal straining that occurs during a pressure-flow study is real or artifactually induced by the surroundings and presence of indwelling catheters. The patient should always be asked to void normally and in as relaxed a way as possible. If the patient has an acontractile detrusor, voiding can be achieved only by straining. If the detrusor contracts during voiding but the patient also strains, then the tracing is more difficult to interpret.
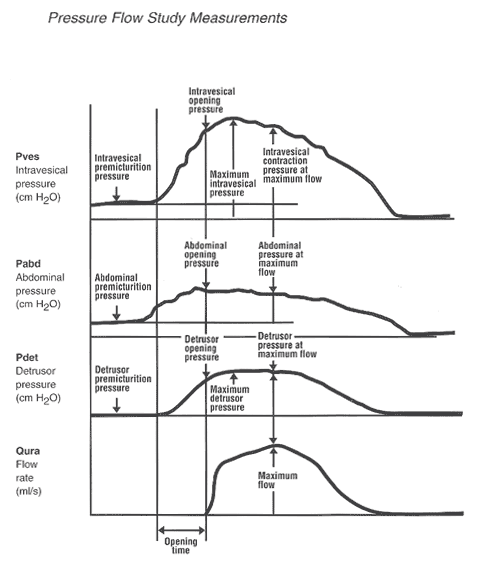
Although pressure-flow studies are an established and accepted urodynamic modality, what constitutes a normal voiding mechanism is incompletely understood, as is the normal range for detrusor pressure during voiding in women. The main clinical use of pressure-flow studies is to document the mechanism of abnormal voiding. The clinical setting in which pressure-flow studies are most useful in women is in the patient who has undergone pelvic surgery and has developed post-operative voiding dysfunction. The dysfunction may be secondary to denervation, resulting in an under-active or acontractile detrusor, or the dysfunction may be secondary to increased outlet resistance produced from the surgery. Pressure-flow studies performed under fluoroscopy can be a useful diagnostic urodynamic procedure. The size of bladder and presence of trabeculations, bladder diverticula, and vesicoureteral reflux can be visualized. Competence of the sphincter can be assessed and the patient's ability to initiate and stop micturition can be observed. The site of significant outflow obstruction usually can also be detected.
Summary:
Any condition that affects contractility or urethral resistance can impair micturition. Uroflowmetry is a simple noninvasive test that can be used to document voiding dysfunction objectively. Because it does not provide direct information on expulsive forces or outlet resistance, it is probably best considered a screening test. Accurate measurement of the urinary flow rate provides important and useful information that may indicate the presence of bladder outlet obstruction. Careful examination of the flow pattern may indicate a possible etiology for an abnormal flow pattern may indicate a possible etiology for an abnormal flow pattern. The uroflow, by itself, can neither diagnose bladder outlet obstruction nor predict which patients will benefit from surgery to relieve obstruction. In view of its limitations, in circumstances in which doubt remains after an uroflow study, further complex urodynamic studies are needed to identify the etiology of voiding dysfunction. Pressure flowmetry provide information on detrusor and abdominal pressure. They are helpful in differentiating voiding dysfunction secondary to obstruction from that secondary to an under-active detrusor. More research is needed to define normal voiding parameters in women and to determine the value of these tests in clinical practice.
Suggested Reading:
- Melville JL, Katon W, Delaney K et al. Urinary incontinence in US women: a population-based study. Arch Inter Med 2005;165:537-542
- Kenton K, Fitzgerald MP, Brubaker K. Striated urethral sphincter activity does not alter urethral pressure during filling cystometry. Am J Obstet Gynecol 2005;192:55-59
- Fallon B, Kreder KJ. Urodynamic assessment of sphincteric function in the incontinent female: which test, and does it matter anyway? Curr Uro Rep 2006;7:399-404
- Pfisterer MH, Griffiths DJ, Schaefer W et al. The effect of age on lower urinary tract function: a study in women. J Am Geriatr Soc 2006;54:405-412
- ACOG Practice Bulletin. Urinary incontinence in women. Number 63, June 2005
- Abrams P, Cardozo L, Khoury S, Wein A. editors. Incontinence, 2nd ed. Plymouth, UK: Health Publication Ltd; 2002. (Level III)
- Weber AM. Leak point pressure measurement and stress urinary incontinence. Curr Womens Health Rep 2001;1:45-52 (Level III)
- Weber AM. Is urethral pressure profilometry a useful diagnostic test for stress incontinence? Obstet Gynecol Surv 2001;56:720-735. (Level III)
- Assessment and treatment of urinary incontinence. Scientific Committee of the First International Consultation on Incontinence. Lancet 2000;355:2153-2158. (Level III)
- Contreras Ortiz O. Stress urinary incontinence in the gynecological practice. Int J Gynecol Obstet 2004;86(suppl):S6-16. (Level III)
Published: 9 February 2009
Dedicated to Women's and Children's Well-being and Health Care Worldwide
www.womenshealthsection.com


