Domestic Violence During PregnancyWHEC Practice Bulletin and Clinical Management Guidelines for healthcare providers. Educational grant provided by Women's Health and Education Center (WHEC). Domestic violence is widely recognized to be a public health issue of epidemic proportions. One in four U.S. women will be abused by an intimate partner during her life-time. In the clinical setting, 35% of obstetrics and gynecology patients, 26% of women seen in primary care practices, and 41% of women presenting to emergency departments report experiencing intimate partner violence at some point in their lives. This violence may include repeated battering and injury, psychological abuse, sexual assault, progressive social isolation, economic deprivation, and intimidation. Various medical professional organizations have recommended that screening for domestic violence be incorporated into routine medical practice. However, significant barriers have inhibited adoption of these recommendations. Physicians practicing in today's fast-paced environment find it more and more difficult to administer all recommended health screenings to their patients. The use of reliable, time-saving, and cost effective screening tools make this a more attainable goal. Domestic violence is an important problem in women's health, with many complications and associated costs. It is estimated that up to 23% (range 0.9 to 23%) of pregnant women are affected by domestic violence (1), and such abuse is associated with unintended pregnancy, increased maternal depression, suicide attempts, and tobacco, alcohol, and drug abuse. Domestic violence may even escalate during pregnancy. Pregnancies affected by domestic violence have an increased incidence of low maternal weight gain, anemia, infection, first/second trimester bleeding, late entry to care, preterm labor, low birth weight, and increased admissions to the normal intensive care unit. Homicide is one of the leading causes of pregnancy-associated death, commonly resulting from intimate partner violence. Many victims of intimate partner violence experience more than one type of violence, and the longer abuse continues, the more likely multiple forms will occur. The purpose of this document is to estimate the prevalence of domestic violence during pregnancy and characteristics of reporting in general and military settings. It promotes the guidelines for screening of domestic violence and various screening tools are discussed. The medical community is uniquely positioned to lessen this impact, at the very least by alleviating the isolation that is often integral to victimization. In accordance with expert guidelines, clinicians should screen all women for partner abuse and provide support and information about available resources for patients identified as victims of violence. Dynamics of Partner Abuse:Intimate partner violence is typically characterized by ongoing, repetitive acts of relatively minor physical assault accompanied by patterns of control, intimidation, and isolation. An abuser may try to control access to money, transportation, modes of communication (e.g., telephone or computer), or even health care (2). An estimated 20% of abused women have partners who interfere with their medical care. Therefore, clinicians should be sure to inquire about intimate partner violence with female patients who do not comply with advice or who delay their care. Intimidation may range from a raised eyebrow to open threats and stalking, and creates an unstable environment in which an abused woman feels she could be assaulted for the most benign action. Isolation may take many forms and serves multiple purposes for the abuser. Separation from friends, family, and coworkers prevents detection of violence, fosters dependence of the woman on her abuser, and robs the victim of any potential means of escape. Most abused women repeatedly seek outside help for the violence they are experiencing but lack the personal or economic resources to gain independence. Indeed, the most dangerous time for a victim can be when is attempting to leave an abusive relationship. World Health Organization (WHO) Multi-country Study on Women's Health and Domestic Violence against Women Study Team (3) conducted surveys in ten countries, revealed for all settings combined, women who reported partner violence at least once in their life reported significantly more emotional distress, suicidal thoughts (2.9 [2.7 -- 3.2]), and suicidal attempts (3.8 [3.3 -- 4.5]), than non-abused women. These significant associations were maintained in almost all of the sites. Between 19% and 55% of women who had ever been physically abused by their partner were ever injured. In addition to being a breach of human rights, intimate partner violence is associated with serious public-health consequences that should be addressed in national and global health policies and programs. Each year in the United States, nearly 5 million domestic physical or sexual assaults occur to nearly 1.5 million women over 18 years of age. Women who are pregnant have a documented rate to abuse during pregnancy of 4% to 20%. In 2005, the Centers for Disease Control and Prevention (CDC) published a report that estimated direct and indirect costs of domestic violence at $ 5.8 billion per year in the United States. Medical and mental health care services accounted for nearly $ 4.1 billion. Annually, 8 million days of lost productivity were attributed to domestic violence (1). These figures probably underestimate, because health care and other costs due to domestic violence are often not recognized or not reported. These figures also do not take into account the cost of health care services sought for other somatic complaints associated with domestic violence, but not directly related to abuse. Women who experience domestic violence, also referred to as intimate partner violence, report poorer health status overall and use health care services more frequently (4). They seek medical care not only for serious injuries, but for a variety of other somatic and psychological complaints. They have more frequent gynecologic, gastrointestinal, chronic pain, and psychiatric complaints. Other common complaints include frequent sexually transmitted diseases (STDs), unwanted pregnancies, pelvic pain, digestive problems, back pain, and depressed mood. Abused women have higher rates of comorbid psychiatric disorders, including mood, eating, and substance abuse disorders. Screening for Domestic Violence:Many major medical organizations recommend routine intimate partner violence screening in all adult women. Because repeated inquiry may increase detection of abuse, guidelines typically encourage periodic screening beyond that performed at the initial patient visit. A number of studies have attempted to identify physician and patient barriers to screening for domestic violence (5). Insufficient time, lack of education, discomfort, and a lack of known effective interventions have been cited as primary barriers for physicians. When physicians do attempt to screen for domestic violence, patients often fail to disclose abuse due to fear, shame, and lack of trust. Combined patient and physician barriers make domestic violence screening complex and challenging. All of the sources agree that screening may still be appropriate in adult patients due to high domestic violence prevalence rates, low cost of screening, and the potential benefit for individual patients. An additional benefit of domestic violence screening may be that, if done appropriately, it can positively affect the patient-physician relationship. When and how to screen: Domestic violence is found across all cultural, ethnic, religious, educational, and socioeconomic backgrounds. However, stereotypes still seem to influence some healthcare providers' decisions about screening. When a patient's history and physical examination are suspicious for abuse, screening for domestic violence is paramount. Although clues may present from the patient's conversation or physical findings, no single symptom or finding is an absolute predictor of domestic violence. Therefore, several organizations and experts recommend screening routinely, not just during health maintenance examination. Because domestic violence is dynamic, screening during successive patient encounters will yield different answers. An answer of "no" to a domestic violence screening question today does not mean it will be "no" in the future. Healthcare provider comfort and dialogue with patients are important prerequisites to effective implementation of screening. In general, it is more appropriate to screen women for abuse after a rapport has been established with the interviewer (6). Screening as part of a women's sexual history, or along with anticipatory guidance questions, would also seem appropriate. Simple and direct clinical inquiry that avoids ambiguity is best. This can be done orally or through the use of questionnaires. It is vital to ensure privacy during administration and completion of questionnaires. The environment in which domestic violence screening occurs is key to its success. Because women in abusive relationships live in a chaotic, violent world, it is important for the screening environment to feel private and safe. Normalizing statements such as "Because violence is so common in women's lives, it is our policy to ask all women about possible violence in their lives" can help make the exchange easier for both the physician and patient. The physician needs to be aware of his/her body language and other non-verbal responses to the information shared. It is crucial to convey that the practitioner is listening and acknowledges the patient's courage in sharing this information. In qualitative studies, women from various cultural groups report that they seek respectful, supportive, non-judgmental, and attentive medical providers to facilitate discussions of abuse (5). 2-year follow up in this study (6) has shown that assistance provided by a domestic violence advocate to women who were in an abusive relationship and spent at least one night in a women's shelter was associated with experiencing less violence over time, a perception of a better quality of life and social support, and less difficulty in obtaining community resources. Screening ToolsOver the last two decades, a number of techniques have been suggested for facilitating domestic violence screening. However, few of these screening tools have been validated against established diagnostic tools such as the Conflict Tactic Scales (CTS), Index of Spouse Abuse (ISA), or the Abuse Risk Inventory (ARI). Thus, the sensitivity, specificity, and predictive value of domestic violence screening tools are often not available. Only one of these tools, the Woman Abuse Screening Tool (WAST), has been studied in more than one patient population (7). Therefore, specific comparisons between domestic violence screening tools are difficult at this time. The Abuse Assessment Screen (AAS):It is the oldest short domestic violence screening tool still used today. The Abuse Assessment Screen (AAS) was developed for the detection of abuse during pregnancy. It consists of five questions, but a short-ended three question version has also been studied. Both the long and short AAS tools have been shown to correlate well with CTS and ISA. However, data regarding sensitivity, specificity, and predictive values have not been reported (6). The tool has been translated into six languages in this publication, and it also includes body maps for documentation of injuries. Abuse Assessment Screen:
MARK THE AREA OF INJURY ON A BODY MAP AND SCORE EACH INCIDENT ACCORDING TO THE FOLLOWING SCALE: 1 = Threats of abuse including use of a weapon If any of the descriptions for the higher number apply, use the higher number. 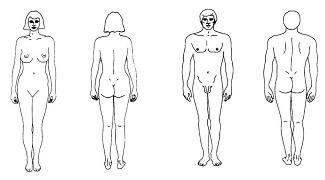 The Hurt, Insult, Threat, Scream (HITS) Screen:The HITS screening tool was designed as a "paper-and-pencil"instrument for identifying both physical and verbal abuse. The four items are scored on a Likert 5-point scale. A score of 10 or greater is considered positive for domestic violence. It has been validated against CTS in a study of 160 female patients in an urban/suburban family practice setting and 99 self identified abused women (6)(7). The HITS scores were strongly correlated with the CTS, with sensitivity and specificity of 96% and 91%, respectively. Positive predictive and negative predictive values in the family practice setting were 87% and 97%, respectively. A verbal form of the HITS questionnaire would probably have similar accuracy. Of note, a woman could deny physical abuse but still screen positive for domestic violence with this tool. Hurt, Insult, Threaten, Screen Tool: How often does you partner:
Answers scored as; 1= never, 2= rarely, 3= sometimes, 4= fairly often, 5= frequently for each of the questions. A total score of ≥ 10 is considered a positive screen for abuse. The Partner Violence Screen (PVS):The Partner Violence Screen (PVS) tool consists of three questions that address physical violence and women's perception of their safety. A positive response to any of the three questions is considered positive for domestic violence. The PVS was tested in 322 women presenting at emergency rooms in two urban hospitals. Both the CTS and ISA instruments were used for validation (8). Because two instruments were used for validation, ranges for sensitivity (64.5% to 71.4%), specificity (80.3% to 84.4%), positive predictive value (51.3% to 63.4%), and negative predictive value (87.6% to 88.7%) were reported. By including questions about past relationships, this screening test takes into account the dynamics of changing relationships. In fact, the highest prevalence of abuse in this study occurred in women who had no current partner and only a previous relationship. Partner Violence Screen Tool:
An answer to any of the above is equal to a positive screen. The Woman Abuse Screening Tool (WAST):The WAST consists of eight questions addressing emotional, physical, and sexual abuse. It has been validated against ARI (8). The first two questions of the tool have been shown in a small population (n = 24) to have a sensitivity and specificity of 91.7% and 100%, respectively. It has been tested in larger population and in Spanish speaking population, it was found to have a lower sensitivity in primary care patients then in self-identified shelter patients. This underscores the importance of studying this and other tools in diverse populations. Woman Abuse Screening Tool:
*Questions 1 and 2 comprise WAST-Short. A score of 1 given to responses of "a lot of tension" and/or "great difficulty" and 0 to the other response. A total score of 1 is considered a positive screen. Establishing A Protocol in Clinical Practice:Administering these tools takes no more than a few minutes. Listening, assessing and providing interventions as necessary will take additional time. The practitioner should consider in advance how disclosure will be handled. Remain aware 5 key points of intimate violence abuse (9):
Utilization of community resources is essential. Allowing abused patients to use private office telephones to speak to domestic violence crisis counselors or law enforcement is especially important if the woman is in immediate danger. Giving a patient a handout with a written telephone number for her to call at a later time may put her at risk, so it is important to always ask first if it is safe to give her that information. Screening for intimate partner violence should be done in a safe, private setting. No other adult known to the patient should be present, and children should be ideally be excused from the room prior to initiating questions about partner-abuse. Clinicians should be aware that in-office language interpreters may come from the patient's community and therefore could pose a potential threat to open communication with the patient. Use RADAR to recognize and teat victims of abuse (10): Remember to ask routinely about intimate partner violence; Safety Assessment and Safety Planning:When a patient reveals that she is being abused, the clinician should validate her experience by telling her she is not alone and no one deserves to be abused. Brief statements of empathy and validation can be powerful interventions (11). The clinicians should then perform a quick safety assessment by establishing if the batterer has a weapon or has ever threatened to kill the patient and if the patient feels she is in any immediate danger. Inquiring about the first, the most recent and most severe episode of abuse is helpful in assessing whether the violence is escalating. The clinician should also ask specifically about the types of abuse and whether the patient has ever sought medical treatment or attempted suicide. After intimate partner violence has been disclosed, the patient's experience validated, her safety assessed, and referrals made, the clinician should review a "quick-escape" plan in the event that the patient ever needs to flee immediately or decides to leave her abusive situation permanently. Specifically the patient should be encouraged to identify places she could go if she were in imminent danger (e.g., friends, family, shelter) and to make copies of important personal and family documents such as driving licenses, passports, pay stubs, birth certificates, and immunization records. She should also make note of Social Security, bank account, and credit card numbers. The patient should place these documents and numbers in a plastic bag along with a change of clothes for her and her family, and if possible, an extra set of car keys. This bag may be hidden outside the home for use in the event she ever decides to escape. Referrals: Healthcare provider who has identified intimate partner violence should provide the patient with information about available resources such as telephone numbers of hot-lines, shelters, local support groups, and legal aid services. In the U.S., a nation-wide domestic violence hot-line exists with trained operators who can offer aid and direct callers to local resources (1-800-799-SAFE). Additionally, each state has a domestic violence coalition that abused women can call to find services in their area. Clinicians may obtain useful informational materials such as posters and pamphlets from these state-wide coalitions. Such material can be displayed in the office waiting and exam rooms to serve as patient resources as well as cues that the clinical environment is a safe place to discuss about the violence in their lives. When providing resource information, clinicians should be certain their patients are able to use them. Many materials are available in languages other than English and for patients with low literacy. Additionally, clinicians should be aware that take-home materials about intimate partner violence could pose a threat if discovered by an abuser. If there is concern about discovery, then information taken out of the doctor's office must look innocuous. Documentation and Mandatory Reporting:The patient's medical record may someday aid in prosecuting her abuser in a court of law. To that end, it is important that the clinician document a description of the abuse as recounted by the patient and take particular care to state the identity of the abuser (e.g. husband, boyfriend). If a clinician suspects abuse but the patient does not disclose it, this suspicion should be noted in the patient's chart. Counseling for intimate partner violence is a clinical activity that may be coded on charge sheets for insurance billing purposes (995.81, 995.82, 995.83, V61.11). However, prior to billing, the clinician should discuss with the patient whether the abuser has access to insurance statements. These documents might reveal that the victim has disclosed her abuse and could potentially put her at risk. Most states do not require health care providers to report of intimate partner violence to law enforcement unless injury has been inflicted by a gun or knife (9). If health care providers are uncertain about their local reporting requirements, they may contact their local domestic violence coalitions for clarification. Domestic Violence in Pregnant Military Population:The military environment possesses a unique set of circumstances and stressors that may directly affect family violence. These include periods of family separation, tensions between the demands of duty and the demands of family life, stress related to the military mission, frequent relocation, perceived dangers associated with military training and combat, as well as financial stressors (12). Although it has been suggested that the prevalence of domestic violence may be higher in a pregnant military population, this has not been studied extensively. In studies comparing the non-pregnant military population with the civilian population, two studies have shown higher rates of physical spousal abuse in the military, whereas another study showed similar prevalence rates of abuse between army and civilian samples after controlling for age and race. However, the abuse among military service members was more severe than their civilian counterparts (12). In a recent study (13) a total of 1,162 women were screened for domestic violence between January 2007 and March 2008. The prevalence of domestic violence in this single study of a pregnant population presenting for prenatal care at the largest U.S. military treatment facility in the Department of Defense was 14.5%. This is in the upper range of prevalence of domestic violence in pregnancy reported in the non-military literature (0.9-23%). Additionally, in this population, unmarried status and poor history of abuse may indicate a higher risk of abuse. With the increased stressors and demands placed on the military service members and their families during wartime, this is an especially important area for future research. Further studies with multiple screenings throughout pregnancy may identify a higher prevalence of abuse in the pregnant military population. The importance or routine screening in pregnant women is essential. Unmarried women and women with a history of abuse also may be at greater risk. Often victims need to be asked about domestic violence several times before they are comfortable enough to disclose abuse or identify their experiences as abuse. Intimate Partner Violence and Postpartum Depression:The Pregnancy Risk Assessment Monitoring System (PRAMS) is an ongoing population-based public health surveillance project that collects self-reported information on maternal attitudes and experiences before, during and after delivery of a liveborn infant. The PRAMS mental health module measures depressive symptoms with 2 questions, each with ordinal response categories. The first question measured depressed mood by asking, since the new baby was born "How often have you felt down, depressed, or hopeless?" the second question measured anhedonia by asking, "How often have you had little interest or little pleasure in doing things?" Women were asked to report "always", "often", "sometimes", "rarely", or "never". Mothers who said "always" or "often" to either question or "sometimes" to both questions are classified as experiencing symptoms of maternal depression. A controlling partner is the only factor among those factors that were examined in preliminary analysis that had a statistically significant association with persistent depression. In this study (14) experiencing a controlling or threatening partner was reported by 6.2% of mothers. Occasional or frequent symptoms of maternal depression was experience by 23% in this group of mothers of newborn and almost one-half of these mothers continued to experience symptoms of depression 2 years later. Clinicians who provide postpartum care should recognize the importance of screening and appropriate treatment for maternal depression and psychological abuse from a partner. Screening for a controlling or threatening partner among women with even mild postpartum depression may identify those who are at higher risk for long-term depression. Future research with a more robust sample size is needed to confirm the association between reporting a controlling partner and persistent maternal depression and to assess the implications of this relationship. Poor interpersonal relationships may be more highly related to persistent depression that incident depression. Other factors that are usually identified to be associated with persistent maternal depression are fair or poor health, low education, high anxiety, and a history of childhood sexual abuse. Summary:Intimate partner violence affects 1 out of 4 women in the US and has a tremendous effect on the health and well-being of female patients. The medical community is uniquely positioned to lessen this impact, at the very least by alleviating the isolation that is often integral to victimization. In accordance with expert guidelines, clinicians should screen all women for partner abuse and provide support and information about available resources for patient identified as victims of violence. Domestic violence is a multifaceted problem with high prevalence and substantial costs to society. Using these time-saving screening tools can facilitate discussion of abuse. However, it is important to note that a positive screen with any of the tools demands further evaluation. On recognition of ongoing domestic violence, assessment of safety and referral to appropriate resources are essential. The objective of screening is to aid in the identification of a significant problem for which an effective intervention is available. These screening tools discussed above are good starting points, but more comparative studies in different populations are needed. These interventions have not been proved effective in either preventing or treating abuse. Nonetheless, although solid intervention studies with objective outcomes measurements are lacking in the field of domestic violence, some evidence suggests that interventions can be effective. A team approach in which practitioners, office staff, mental health professionals, law enforcement, and advocacy groups work together is needed to effectively intervene in this complex and challenging problem. Acknowledgment:Special thanks to LT Monica A. Lutgendorf, MC USN, Department of Obstetrics and Gynecology, Naval Medical Center Portsmouth, Portsmouth, VA (USA) for her assistance in preparing the manuscript and sharing her research. We look forward to develop this essential service with US Military. Funding:The project was funded by WHEC Initiative for Global Health. References:
|