Vieillissement en santé: un appel à l'action mondialeBulletin WHEC pratique et de directives cliniques de gestion pour les fournisseurs de soins de santé. Subvention à l'éducation fournie par la santé des femmes et de l'Education Center (WHEC). Population ageing is having profound effects on societies all over the world. It is a quiet, almost unseen social revolution. The 21st century offers a bright vision of better health for all. It holds the prospect not merely of longer, but superior quality of life, with less disability and disease. It is time to realize that ageing and health is a global issue; it should be considered as an essential component of the continuing globalization process that is reshaping our world. It should be included in the growing interaction between countries that currently exists in terms of world trade, services, foreign investment and capital markets. Investing in health across the lifespan and their environment is a prerequisite for sustainable development. As women live longer than men, the quality of their longer life becomes of central importance. Primary prevention strategies will be most effective when initiated as early as possible. As the evidence shows, the loss of ability typically associated with ageing is only loosely related to a person's chronological age. There is no "typical" older person. The resulting diversity in the capacities and health needs of older people is not random but rooted in events throughout life course that often can be modified, underscoring the importance of a life-course approach. The purpose of this document to discuss physiology, biochemistry, immunology and management of the ageing process. Ageing is the progressive accumulation of changes with time that are associated with or responsible for the ever-increasing susceptibility to disease and death which accompanies advancing age. These time-related changes are attributed to the ageing process. Societies that adapt to this changing demographic and invest in Healthy Ageing can enable individuals to live both longer and healthier lives and for societies to reap the dividends. IntroductionPopulations around the world are rapidly ageing. Ageing presents both challenges and opportunities. It will increase demand for primary health care and long-term care, require a larger and better trained workforce and intensify the need for environments to be made more age friendly. It is not unreasonable to expect on the basis of present data that the healthy life span can be increased by 5-10 years by keeping body weight down, at a level compatible with a sense of well-being, while ingesting diets adequate in essential nutrients but designed to minimize random free radical reactions in the body. Today, for the first time in history, most people can expect to live into their 60s and beyond. This reflects our successes in dealing with fatal childhood disease, maternal mortality, and more recently, mortality in older ages. When combined with falls in fertility rates, these increases in life expectancy are leading to equally significant changes in population structure population ageing (1). One crucial consequence is that in older age the people with the greatest health needs tend to also be those with the least access to the resources that might help to meet them. This association has major implications for policy, which will need to be crafted in ways that overcome, rather than reinforce, these inequities. It is essential that the potential social and economic impacts of improved life expectancy are fully appreciated and acted upon today. The well-being of society depends on the good health of its older members in their later years. For policymakers and individuals alike, this means planning for the future. The world is learning how to grow old successfully. The Global ChallengeAccording to the World Health Organization (WHO) by 2050, 1 in 5 people will be 60 years or older. The global population aged over 65 is increasing by 750,000 a month. A child born in Japan today can expect to live to be 80 years old. By 2025, there will be more than 800 million older people in the world, two-thirds of them in developing countries, and a majority of them will be women (2). Increases in the older population by up to 300% are expected in may developing counties, especially in Latin America and Asia, in the next 30 years. There will be 374 million people over the age of 60 in China alone more than the total present population of the United States. It has been estimated that by the year 2025, the number of older people older than 60 years in the planet will exceed 1 billion and 2 billion by the year 2050 (4). At present 15% of the population of the United States is aged 65 and above, compared to 4% at the beginning of the 20th century. Although the population is ageing more slowly in industrialized countries, these countries will have relatively more people in the "oldest old" bracket. For example, there were only 200 people aged 100 years in France in 1950. By the year 2000, the number has risen to 8,500 and by 2050 it is projected to reach 150,000 - a 750-fold increase in 100 years of age. The global challenge of ageing is made more complex by other demographic changes that are occurring simultaneously. In the next 25 years, the population aged 65 and above is likely to grow by 88% compared to an increase of 45% in the working age population (3). This implies that a steadily declining number of people of reproductive age will have to provide for an expanding number of dependents, not merely in the form of direct support to older relatives but also through taxation, the provision of health and social services and social security. In 2017, there were an estimated 962 million people aged 60 years or older worldwide, that is, around 13% of the global population. This part of the population is growing at an annual rate of about 3% and further growth is almost inevitable (3). An increasing part of this population lives in cities, where the combination of urbanization and ageing leads to new public health challenges, such as a higher risk of mental disorders, resulting in impairments in the ability to function socially. However, while cities pose major challenges for older citizens, they also offer opportunities for the implementation of policies and interventions that promote public health. Definition - What is ageing?In 1991, the book Evolutionary Biology of Ageing offered the following definition of ageing: "a persistent decline in the age-specific fitness components of an organism due to internal physiological deterioration" (5). Healthy Ageing is defined by the World report on ageing and health as the process of developing and maintaining the functional ability that enables well-being in older age. Functional ability is determined by the person's intrinsic capacity (the combination of all the individual's physical and mental capacities), relevant environmental factors, and the interaction between the two. Environmental factors include policies, systems, and services related to transport, housing, social protection, streets and parks, social facilities, and health and long-term care; politics; products and technologies; relationships with friends, family, and caregivers; and cultural and social attitudes and values. Health Characteristics in Older AgeGiven the complexity of intrinsic capacity and functional ability of the second half of life, this discussion highlights key issues that can provide a frame for understanding health trends in older age. At a biologic level, ageing is characterized by a gradual, lifelong accumulation of molecular and cellular damage that results in a progressive, generalized impairment in many body functions, an increased vulnerability to environmental challenges and a growing risk of disease and death (6). Movement Function: After a peak in early childhood, muscle mass tends to decline with increasing age, this can be associated with declines in strength and musculoskeletal function (7). One way of measuring muscle function is to measure hand grip strength, which is a strong predictor of mortality, independent of any disease-related mortality, independent of any disease-related influences. Women tend to have weaker grip strength than men, and for both sexes' strength declines with increasing age. The rate of deterioration of grip strength was similar across most of the countries studied (8). However, the peak level reached varies markedly, with people in India and Mexico generally having lower strength across all ages and sexes (8). These differences may reflect a mix of genetics and early-life factor, such as nutrition. Ageing is also associated with significant changes in bones and joints. With age, bone mass, or density, tends to fall, particularly among postmenopausal women. This can progress to a point where the risk of fracture is significantly increased ( a condition known as osteoporosis), which has serious implications for disability, reduced quality of life and mortality. Hip fractures are particularly devastating type of osteoporotic fracture, and as a result of population ageing, they will become more common, reaching an estimated annual global incidence of 4.5 million in 2050 (9). Articular cartilage undergoes significant structural, molecular, cellular and mechanical changes with age, increasing the vulnerability of the tissue to degeneration. As cartilage erodes and fluid around the joint decreases, the joint becomes more rigid and fragile. Regular moderate physical activity has been shown to improve the biomechanical and biological properties of articular cartilage. These and other age-related declines ultimately impact on broader musculoskeletal function and movement. This is reflected in a decrease in gait speed that is, the time someone takes to walk a specific distance. Gait speed is influenced by muscle strength, joint limitations and other factors, such as coordination and proprioception, and has been demonstrated to be one of the most powerful predictors of fracture outcomes in older age (10). Sensory Functions: Ageing is frequently associated with declines in both vision and hearing, although there is marked diversity in how this is experienced at an individual level. Age-related hearing loss (known as presbycusis) is bilateral and most marked at higher frequencies. It results from cochlear ageing; environmental exposures, such as noise; genetic predisposition; and increased vulnerability from physiological stressors and modifiable lifestyle behaviors (11). Worldwide, more that 180 million people older than 65 years have hearing loss that interferes with understanding normal conversational speech (12). Age is also associated with complex functional changes in the eye that result in presbyopia, a decrease in focusing ability that leads to the blurring of vision, which often becomes apparent in mid-life. Another common change associated with ageing is increasing opacity of the crystalline lens, which can ultimately result in cataract. The age of onset, rate of progression and level of reduced vision vary significantly among individuals, reflecting genetic patterns and environmental exposure (12). Ageing is also strongly associated with age-related macular degeneration, which causes retinal damage and leads rapidly to severe visual impairment. It is highly prevalent in people older than 70 years, and a leading cause of blindness in high-income and upper-middle-income countries. Cognitive Functions: They vary greatly among people and is closely related to years of education. Many cognitive functions begin to decrease at a relatively young age, with different functions decreasing at different rates. As a consequence, functioning becomes increasingly heterogeneous with increasing age (13). Some deterioration in memory and the speed of information processing is common, and complaints about it are frequently reported by older people. However, although ageing is associated with a decrease in the capacity to tackle complex tasks that require dividing or switching attention, it does not appear to reduce the capacity to maintain concentration or to avoid distraction. Similarly, although ageing is associated with reduction in the capacity to learn and master tasks that involve active manipulation, reorganization, integration or anticipation of various memory items, there is little association with memory for factual information, knowledge of words and concepts, memory related to personal past, and procedural memory (14). Thus, not all cognitive functions deteriorate with age, and language features, such as comprehension, reading and vocabulary, in particular remain stable throughout life. The variation from person to person in the decline in cognitive functions with age influenced by many factors, including socioeconomic status, lifestyle, the presence of chronic disease and the use of medication, suggesting there are opportunities for public-health interventions across the life course. There is also some evidence that normal age-related cognitive decline can be partially compensated for by practical competence and experience acquired through a lifetime and reduced by mental training and physical activity (15). Crucially, the subtle and heterogenous changes in cognitive functioning that are observed in healthy older people are quite distinct from the changes associated with dementia. Sexuality: Although the data on sexual activity in older age are limited, particularly from lower-income countries, population surveys repeatedly show that people often remain sexually active well into advanced age. In one longitudinal study, 73% of participants aged 57-64 years, 53% aged 65-74, and 26% aged 75-85 were sexually active. In oldest age group, 23% of sexually active participants reported having sex once a week or more (16). In line with predominant sociocultural attitudes, the research on these vulnerabilities and sexual dysfunctions rather than on positive aspects of sexuality (16). A recent survey of middle-aged and older people in 29 countries identified the most common dysfunctions among women as a lack of sexual interest (21%), inability to reach orgasm (16%) and lubrication difficulties (16%). Among men, the most common dysfunctions appeared to be difficulty in achieving or maintaining an erection (37%), lack of interest in sex (28%), climaxing too quickly (28%), anxiety about performance (27%) and an inability to climax (20%) (17). Despite these challenges, or with the assistance of widely available medical treatments, sexuality remains important in older age and takes many forms. One often overlooks the subject of sexual dysfunction in older people living in a care home or institutions. This is a complex issue touching on both the rights of these older people to express their sexuality and the need to protect vulnerable individuals from predatory behavior. Particular ethical dilemmas may arise in relation to sexuality and dementia. More research and better guidance on how to manage these delicate and complex situations are urgently needed. Immune Function: Particularly T-cell activity, declines with age (18). These changes mean that the capacity to respond to new infections (and vaccination) falls in lager life, a trend known as immunosenescence. There is also some evidence that chronic stress can reduce the immune response and the effectiveness of vaccines in older people, and an age-related increase in serum levels of inflammatory cytokines, known as inflammageing, has been linked to a broad range of outcomes, including frailty, atherosclerosis and sarcopenia. Although precise association of these trends with broader physiological changes associated with ageing is still open for debate, immune function clearly has an important role and may present opportunities for future interventions. This possibility has been reinforced by research in mice suggesting that the effective clearance of senescent cells, another role of the immune system, may delay many disorders related to ageing (19). Functions of the Skin: Skin suffers progressive decrements with age that result from damage caused by physiological mechanisms, genetic predisposition and external insults, particularly sun exposure. Age-related changes at a cellular level can have numerous affects, including a fall in the skin's ability to act as a barrier. The loss of collagen and elastin fibers in the dermis can reduce the tensile strength of the skin, and progressive vascular atrophies can leave patients more susceptible to dermatitis, pressure ulcers and skin tears (20). Combined these changes, may result in older people having an increased susceptibility to many dermatological disorders. Moreover, the cumulative effects of environmental insults, particularly exposure to the sun, contribute to a marked increase in the risk of neoplastic disease. The potential impacts of these changes are not just physical. Many skin conditions can affect individuals' emotional health or lead to changes in the way they are perceived by others; they may also cause withdrawal from social activity, thus preventing full participation in communities and workplaces. Depression and Anxiety: Affective disorders, such as depression and anxiety, tend to occur throughout life in a vulnerable proportion of the population. Episodes of affective disorders might be expected to be more prevalent in older age due to the increased risk of adverse life events. Instead depressive disorders appear to be a little less prevalent among older adults than among younger adults but still affect about 2-3% of older people living in the community (21). However, the prevalence among the most frail and vulnerable older adults living in long-term care facilities is considerably higher, at about 10% (22). Furthermore, compared with the younger adults, older people more often suffer from substantial depressive symptomatology without meeting the diagnostic criteria for a depressive disorder. This condition is often referred to as subthreshold depression and affects nearly 1 in 10 older adults. Subthreshold depression also has a major risk factor for a depressive disorder.The estimated prevalence of anxiety disorders in the older population ranges from 6% to 10%, which is slightly lower than the estimated prevalence of anxiety disorders in younger adults but still represents significant cause of disability (22). The prevalence of anxiety disorders in long-term care facilities has been shown to be somewhat lower and is estimated to be around 5.7% (23). Anxiety disorders and depression often occur together. About 13% of older people with an anxiety disorder also have a depressive disorder, and 36% of older people with depression have a coexisting anxiety disorder. Although affective disorders are prevalent in older people, treatment is often effective, including cognitive behavioral therapy and use of selective serotonin reuptake inhibitors (23). Memory Loss (Dementia): In 2015, dementia affected more than 47 million people worldwide. By 2030, it is estimated that more than 75 million people will be living with dementia, and the number is expected to triple by 2050. This is one of the major health challenges for our time. In an Australian study, it was estimated that around 10% of the expected increase in healthcare costs during the next 20 years would come from demand for care for this condition alone (24). Contrary to popular belief, dementia is not a natural or inevitable consequence of ageing. It is a condition that impairs the cognitive brain functions of memory, language, perception and thought, and that interferes significantly with the ability to maintain the activities of daily living. The most common types of dementia are Alzheimer's disease and vascular dementia. Evidence suggests that the risk of certain types of dementia may be lowered by reducing risk factors for cardiovascular disease. The personal, social and economic consequences of dementia are enormous. Dementia leads to increased long-term care costs of governments, communities, families and individuals, and to losses in productivity for economics. The global cost of dementia care in 2010 was estimated to be US$ 604 billion: 1.0% of global gross domestic product (GDP). By 2030, the cost of caring for people with dementia could be US $ 1.2 trillion or more, which could undermine social and economic development throughout the world. Nearly 60% of people with dementia live in low- and middle-income countries, and this proportion is expected to increase rapidly during the next decade, which may contribute to increasing inequalities among countries and populations. A sustained global effort is thus required to promote action on dementia and address the challenges it poses. No single country, sector or organization can tackle these alone. Towards a dementia plan: a WHO guide provides useful information to Member States for creating and operationalizing a dementia plan (25). This might involve developing a new, stand-alone dementia plan as well as stakeholder mapping and priority setting. The guide seeks to strike a balance between generic recommendations and practical, how-to advice. The Global Dementia Observatory (GDO) is a data and knowledge exchange platform that offers easy access to key dementia data from Member States across the following three domains: policies, service delivery, and information and research. The GDO supports countries in measuring progress on dementia actions outlined in the Global Dementia Action Plan on the Public Health Response to Dementia 2017-2025 and assists them in strengthening policies, service planning and health and social care systems for dementia. Alzheimer's Disease (AD)It is the most common type of dementia. In 2014 as many as 5 million Americans were living with Alzheimer's disease. It is estimated by 2050 this number will increase to 14 million in USA (26). Younger people may get Alzheimer's disease, but it is less common. The symptoms of the disease can first appear after age 60 and the risk increases with age. The number of people living with the disease doubles every 5 years beyond age 65.
Risk factors: Age is the best-known risk factor for Alzheimer's disease. There probably is not one single cause, but several factors that affect each person differently. Family history researchers believe that genetics may play a role in developing Alzheimer's disease. Changes in the brain can begin several years before the first symptoms appear. Researchers are studying whether education, diet, and environment play a role in developing Alzheimer's disease. Scientist are finding more evidence that some of the risk factors for health disease and stroke, such as high blood pressure and high cholesterol may also increase the risk of Alzheimer's disease. There is growing evidence that physical, mental and social activities may reduce risk of Alzheimer's disease. See Healthy Brain Initiatives discussed below in this review. Other Complex Health Issues in Older Age: Older age is also characterized by the emergence of several complex health states that tend to occur only later in life and do not fall into discrete disease categories. These are commonly known as geriatric syndromes (27). The definition of frailty remains contested, but it can be considered as a progressive age-related decline in physiological systems that results in decreased reserves of intrinsic capacity, which confers extreme vulnerability to stressors and increases the risk of a range of adverse health outcomes. Frailty, care dependence and comorbidity are distinct but closely related. Urinary incontinence (that is, the involuntary loss of urine associated with urgency or with effort, physical exertion, sneezing or coughing) is a neglected problem in older people, and a strong predictor of a need for care. It is one of the most common impairments in older age, with prevalence increasing with age and being much higher in women than men in all age groups (28). Falls are a major health problem for older adults. Various reviews and meta-analyses have estimated that 30% of people older than age 65, and 50% of people older than age 85, who live in the community will fall at least once each year (29). HEALTH SYSTEMS & RISING DEMANDBecause the health dynamics of older age are related to increased needs for health care, it might be expected that increasing age would be associated with increased health-care utilization. And given that the burden of disease and declines in capacity are greater in low- and middle-income countries, it might also be expected that this trend would be more marked in low-resource settings. However, evidence indicated that there is a disconnect between healthcare need and health care utilization, both in these settings, and in disadvantaged subgroups of older people in high-income settings. Economic impact of population ageing on health systems: Will the benefits of the investments in health and well-being of older people be outweighed by the health-care costs of a longer life? What overall impact will population ageing have on healthcare expenditure? For many reasons it is extremely difficult to predict the impact that population ageing will have on healthcare expenditures. First, although older age is generally associated with an increased need for care, the link between the need for care and utilization is weak. Even in high-income countries, poorer older people, who generally have greater needs, tend to use services less often that their more financially secure peers (30). Second, even if these inequalities in demands for healthcare were overcome and overall demand increased to better match needs, the link between age and healthcare expenditures is not linear. The integration of healthcare and long-term care services will be crucial to maintaining the functional ability and dignity of older people at this stage of life. Care coordination has been shown to be beneficial, and care plans help prevent unnecessary hospital admissions, ensure there are links with long-term care services, and support people to remain at home. Health financing alignment with Healthy Ageing goals: Health-financing policies should be aligned with goals for universal health coverage of ageing population. Practically speaking, health-financing policies encompass raising revenues, pooling and allocating funds, and determining the way in which services are purchased. Particular attention will be needed to ensure not only adequate remuneration for health workers providing care to ageing populations but also to ensure there are appropriate incentives, especially for those working in community-based and primary healthcare settings. Financial incentives can support efforts to encourage health workers to practice in underserved areas and are increasingly used in the health sector in conjunction with salaried and free-for-service arrangement. Although transforming health systems requires action on several fronts, three key themes emerge as priorities:
The Growing Need for Long-Term CareSurvey data have revealed that a significant proportion of older people are care-dependent, and the prevalence increases with age. There is marked variation among countries, ranging from less than 5% of the population aged 65-74 years in Switzerland being care-dependent to around 50% of people of same age in many low- and middle-income countries (depending on how it is measured). Among people older than 74 years, the prevalence is even higher. Global population ageing will significantly increase the absolute number of older people who are care dependent. Financing long-term care: In many countries, discussions about long-term care focus on the sustainability of current financing arrangements in the face of rapidly growing demand. Moreover, informal care is rarely included in estimates of the costs of long-term care. These non-government costs can be substantial and include the costs of unpaid labor and forgone educational and income-earning opportunities for family caregivers and cash payments made by older people or their families for private care. Where long-term is not available, other costs are likely to arise from inappropriate use of acute healthcare services. Thus, although government expenditures on long-term care may appear to be low, these are likely to have been shifted, at least in part, to the health sector. Moving towards an integrated system: A Revolutionary Agenda Changes need to encompass two broad areas. First, long-term care must be recognized as a public good both societally and politically. The enormous social and economic costs of neglecting this challenge also need to be acknowledged. Second, long-term care must be redefined. Instead of thinking about long-term care as a minimal and basic safety net that provides rudimentary support to older people who can no longer look-after themselves, perceptions must shift towards a more positive and proactive agenda. Within this new framework, long-term care must be oriented towards both optimizing intrinsic capacity and compensating for a lack of capacity at a level that maintains an older person's functional ability and ensures dignity and well-being. More broadly, long-term care must promote social cohesion and gender justice, and ensure an acceptable level of well-being for all members of society, including not only dependent older people but also those who care for them. Achieving these goals in an equitable, sustainable and socially just manner is likely to require fundamental shifts in models of national development. These need to reflect the crucial role of long-term care in maintaining social cohesion, the opportunities and economic growth that can accompany reform, and the rights of vulnerable older people. Innovative Assistive Health Technologies can Enable Ageing in Place Innovative assistive health technologies for long-term care - such as remote monitoring and robotic caregivers, have received a great deal of attention. They are often presented as highly promising means for enhancing the functional ability of older people who have declines in their intrinsic capacity, for improving their quality of life as well as that of their caregivers, and for potentially reducing individual and societal costs and enabling ageing in place (31). The reality of innovative assistive health technologies is more nuanced. Solid research on the impact of various devices and interventions is scare, and new technologies can present threats to older people's privacy and autonomy if they are not deployed in a considered and person-centered manner. Notwithstanding the need for more research, the use of particular types of innovative technologies should be based on the needs and preferences of the older person or their caregiver. For example, using tracking and tracing technology might be a good solution for someone with early dementia who wants to walk independently in their neighborhood. During the later stages of dementia, however, this technology might not offer the same advantages and a different approach would need to be used. Several additional ethical issues related to the use of innovative assistive health technologies bear consideration. The impact of innovative technologies on older people's privacy, autonomy and social participation must always be considered. Certain forms of innovative technologies might have the unintended effect of isolating older people or restricting their freedom of movement. These potential harms must be weighed against the benefits on a case-by-case basis. Nonetheless, research indicates that older people have few ethical objections to using innovative technologies and often view them as an acceptable alternative to a lack of care or institutionalization (32). Multiple stakeholders should be involved in developing sound policies for the use of innovative assistive health technologies. Policymakers, care providers, members of industry and academia, and importantly, older people must be involved in policy development. Technologies need to be developed that reflect the needs and preferences of their end-users; and training for caregivers, health professionals and others is crucial. Finally, developing financing mechanisms for research and development, and to ensure equitable implementation requires careful attention, especially in lower-income countries. The main lessons from the experience of the Women's Health and Education center (WHEC) are as follows:
Key benefits of acting on long-term care
Countries have considerable scope for diversity, innovation and flexibility in deciding how to act in these areas. In all countries, a wide range of stakeholders will likely be involved in the process. But only governments can establish and steward long-term care systems as a whole. ACTION PLAN on Ageing and HealthThe process of Healthy Ageing argues that all sectors share a common goal: to build and maintain functional ability. Our initiatives are structured around five key domains of functional ability that are essential for older people to:
Ensuring functional ability in older people is important in addressing population ageing. Relevant to all countries is the consideration of older people's abilities, which emphasizes personal and environmental resources as well as intrinsic capacity. Placing emphasis on maximizing functional ability supports governments, civil society and other partners in increasing their focus on results and impacts. WHEC focuses on these three key areas and cross cutting issues in its initiatives:
Engendering change requires collaborating across various levels of government and among government and nongovernmental actors, including, for example, academics and older people's organizations. Actions that can support intersectoral action on Healthy Ageing include:
Our action plan is designed to enhance different domains of abilities and encourages different sectors to encourage functional ability. In times of heighted concerns over the implications of population ageing, increased national austerity and scarce aid dollars, the focus on abilities provides a way for all sectors at all level of government to decide together how to most efficiently add health to years. HEALTHY BRAIN INITIATIVESThe role of public health in enhancing the physical health of older adults is well known. Public health's role in maintaining cognitive health, a vital part of Healthy Ageing and quality of life, is emerging. The need for a clearly delineated public health role comes at a critical time given the dramatic ageing of the world's population, scientific advancements in knowledge about risky behavior (e.g. lack of physical activity, uncontrolled high blood pressure) related to cognitive decline, and the growing awareness of the significant health, social, and economic burdens associated with cognitive decline. The Healthy Brain Initiative of the Women's Health and Education Center (WHEC) is a multifaced approach to cognitive health with several components, including:
Cognitive decline, ranging from mild cognitive impairment to dementia, can have profound implications for an individual's overall health and well-being. Cognition is a combination of mental processes that includes the ability to learn new thing, intuition, judgment, language, and remembering. The four main domains of public health action items are: monitor and evaluate; educate and empower the nation; develop policies and mobilize partnerships; and assure a competent workforce.  What is dementia?Dementia is a syndrome that can be caused by a number of progressive illnesses that affect memory, thinking, behavior and the ability to perform everyday activities. Alzheimer's disease (AD) is the most common type of dementia. It is an umbrella term used to describe a decline in memory or brain function that impacts and individual's daily life. This is different from the normal decrease in short-term memory most people experience with age. Types of Dementia
Reducing Stigma: Dementia mainly affects older people, although there is growing awareness of cases that start before the age of 65. After age 65, the likelihood of developing dementia roughly doubles every five years. Stigma is an attribute, behavior or reputation which is socially discrediting in a particular way. It causes an individual to be mentally classified by others in an undesirable, rejected stereotype rather than in an accepted, normal one. Identifying stigma is important because 36 million people have dementia worldwide. We believe that more understanding and awareness of the personal perspective would reduce negative connotations, lead to societal empathy, reduce fear and therefore reducing stigma. Seven Stages of DementiaOne of the most difficult things about dementia is that, in most cases, dementia is irreversible and incurable. However, with an early diagnosis and proper care, the progression of some forms of dementia can be managed and slowed down. The cognitive decline that accompanies dementia conditions does not happen all at once. The progression of dementia can be divided into seven identifiable stages: Stage 1: No Cognitive Decline. It can also be defined as the normal functioning stage. At this stage of dementia, a patient does not exhibit any significant problems with memory, or any cognitive impairment. Stages 1-3 of dementia progression are generally known as "pre-dementia" stages. Stage 2: Age Associated Memory Impairment. This stage features lapses of memory most frequently seen in forgetting where one has placed an object and forgetting names that were once very familiar. At this stage, signs are still virtually undetectable through clinical testing. Concern for early onset of dementia should arise with respect to other symptoms. Stage 3: Mild Cognitive Impairment. Clear cognitive problems begin to manifest in stage 3. A few signs of stage 3 dementia include getting lost easily; noticeably poor performance at work, forgetting the names of family members and close friends, difficulty retaining information read in a book or passage, losing and misplacing important objects and difficulty concentrating. Patients often start to experience mild to moderate anxiety as these symptoms increasingly interfere with day to day life. Stage 4: Mild Dementia. Behavior to look for include decreased knowledge of current and/or recent events, difficulty remembering things about one's personal history, decreased ability to handle finances, arrange travel plans, etc., disorientation and difficulty recognizing faces and people. In stage 4 dementia, individuals have no trouble recognizing familiar faces or traveling to familiar locations. However, patients in this stage will often avoid challenging situations in order to hide symptoms or prevent stress or anxiety. Stage 5: Moderate Dementia. Patient need some assistance in order to carry out their daily lives. The main sign of stage 5 dementia is the inability to remember major details such as the name of a close family member or a home address. Patients may become disoriented about the time and place, have trouble making decisions, and forget basic information about themselves, such as telephone number or address. Patients usually do not need assistance with basic functioning such as using the bathroom or eating. Patients also still have the ability to remember their own names and generally the names of spouses and children. Stage 6: Moderately Severe Dementia. When patient begins to forget the names of their children, spouse, or primary caregivers, they are most likely entering stage 6 of dementia and will need full time care. In the sixth stage, patients are generally unaware of their surroundings, cannot recall recent events, and have skewed memories of their personal past. Caregivers and loved ones should watch for delusional behavior, obsessive behavior and symptoms, anxiety, aggression, and agitation and loss of willpower. Patients may begin to wander, have difficulty sleeping, and in some cases will experience hallucinations. Stage 7: Severe Dementia. Along with loss of the motor skills, patients will progressively lose the ability to speak during the course of stage 7 dementia. In the final stage the brain seems to lose its connection of the body. Severe dementia frequently entails the loss of all verbal and speech abilities, loved ones and caregivers will need to help the individual with walking, eating and using the bathroom. By identifying the earliest stages of dementia as they occur, you may be able to seek medical treatment quickly and delay the onset of later stages. Though most cases of dementia are progressive, some may be reversible, and sometimes dementia-like conditions may be causes by treatable underlying deficiencies or illnesses. The more aware you are of these stages, the quicker you will be able to react and seek help, either for yourself or for a loved one. TreatmentsUnfortunately, most dementia related conditions cannot be cured. For most types of dementia, there is no way to slow or reverse cognitive impairment. There are medications and alternative treatments that are used to improve and alleviate symptoms. Treatments and medication will depend heavily on the specific dementia condition in question. Current research suggests that exercise, diet, smoking, cardiovascular disease, cholesterol, diabetes, and mild cognitive impairment may all factor into development of dementia. Making healthy lifestyle choices, especially during middle age, may be integral to dementia prevention. Preventive measures include:
Medications for reversible dementias Some reversible dementias exist, for example, vitamin B12 deficiency can cause pernicious anemia, leading to dementia that can be treated by addressing the deficiency. Medication and supplements that can be treated by addressing the deficiency. Medications and supplements that can completely cure reversible dementias include: Vitamin B12 supplements for pernicious anemia; hormonal supplements for hyperthyroidism, hypothyroidism, or other metabolic imbalances; selective serotonin reuptake inhibitors (SSRIs) or other antidepressants for depression symptoms which may mimic dementia; and antibiotics or medications to treat brain infections like encephalitis or meningitis. Medications for managing dementia symptoms When dementia cannot be treated, slowed or reversed, physicians and medical professionals focus on medications that can make living with dementia easier and more manageable. There are several classes of medications proven to work at treating symptoms and reducing the effects of dementia, which include (33):
Therapy Research has shown that therapy improves well-being, day-to-day functioning, and overall mood in dementia sufferers. Cognitive stimulation therapy, behavioral therapy, reality orientation therapy and validation therapy can be beneficial based on situation. The Montessori educational system, to date largely implemented primarily in early childhood education, is being explored as a possible means of grounding dementia patients; giving them a social, interactive environment that can simultaneously soothe them and encourage active mental engagement. The realities of Alzheimer's disease (AD) and overcoming stigmaThere are two types of AD:
AD is also the leading cause of dementia, accounting for 50% to 80% of cases. For the less than 5% of people with AD who have early-onset Alzheimer's, however, the development of the disease has often been linked to genetics, though it is not always the case. Also, healthy life-style choices, such as regular physical activity, a good diet and continuous mental stimulation, have been known to reduce the risk of development. AD is an irreversible, progressive brain disorder that slowly destroys memory and thinking skills and eventually, the ability to carry out the simplest tasks. It is the most common cause of dementia in older adults. While dementia is more common as people grow older, it is not a normal part of ageing. Capitalizing on recent advances in neuroimaging and genetic biomarker research, scientists have been able to identify specific pathways by which tau- and beta-amyloid, two proteins that are hallmarks of AD, accumulate in the brain over time. The NIA-supported researchers also found that the patterns of tau- and beta-amyloid accumulation were related to specific genetic profiles, providing better understanding of AD risk and possible new avenues for diagnosis and monitoring of the disease (34). AD is a complex, and it is unlikely that any one drug or other intervention will successfully treat it. Current approaches focus on helping people maintain mental function, manage behavioral symptoms, and slow down the symptoms of disease. Most medications work best for people in early or middle stages of Alzheimer's, for example, they can slow down some symptoms, such as memory loss, for a time. It is important to understand that none of these medications stops the disease itself. 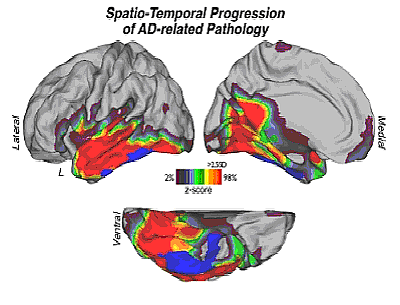  Treatment for Mild to Moderate Alzheimer'sMedications called cholinesterase inhibitors are prescribed for mild to moderate AD. These drugs may help reduce some symptoms and help control some behavioral symptoms. The medications are Razadyne (galantamine), Exelon (rivastigmine), and Aricept (donepezil). Scientist do not understand how cholinesterase inhibitors work to treat AD, but research indicates that they prevent the breakdown of acetylcholine, a brain chemical believed to be important for memory and thinking. As AD progresses, the brain produces less and less acetylcholine; therefore, cholinesterase inhibitors may eventually lose their effect. No published study directly compares these drugs. Because they work in a similar way, switching from one of these drugs to another probably will not produce significant different results. However, an AD patient may respond better to one drug than another. Treatment of Moderate to Severe Alzheimer'sA medication known as Namenda (memantime), an N-methyl D-aspartate (NMDA) antagonist, is prescribed to treat moderate to severe AD. This drug's main side effect is to decrease symptoms, which could allow some people to maintain certain daily functions a little longer than they would without the medication. Namenda may help a person in the later stages of the disease maintain his or her ability to use the bathroom independently for several more months, a benefit for both the person with AD and caregivers. |