Эбола Вирус болезни и беременность
Бюллетень WHEC Практика и клинической управления для медицинских работников. Образовательный грант предоставляемых Здоровье женщин и центр образования (WHEC).
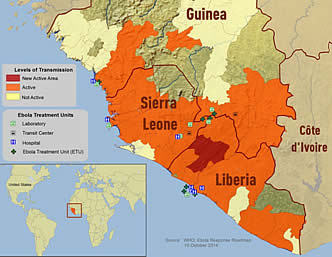
West Africa is currently in the midst of the largest Ebola virus disease (EVD) outbreak in history. As of August 22, 2014, 2,252 people have confirmed or suspected EVD and 1,427 have died in Liberia, Sierra Leone, Guinea, and Nigeria and the outbreak is expected to take a long period of time to control (1). World Health Organization (WHO) declared the current Ebola outbreak a Public Health Emergency of International Concern and working with governments, UN agencies and international and non-governmental organizations (NGOs) partners for several months to respond to this global crisis. A total of 9,216 confirmed, probable, and suspected cases of EVD have been reported in seven affected countries (Guinea, Liberia, Nigeria, Senegal, Sierra Leone, Spain, and the United States of America) up to the end of 14 October 2014. There have been 4,555 deaths. A second EVD-negative sample was obtained from the single confirmed case in Senegal on 5 September (42 days ago). WHO officially declares the Ebola outbreak in Senegal over. Following the WHO Ebola Response Roadmap structure, country reports fall into two categories: 1) those with widespread and intense transmission (Guinea, Liberia, and Sierra Leone); and 2) those with an initial case or cases, or with localized transmission (Nigeria, Senegal, Spain, and the United States of America). An overview of the situation in the Democratic Republic of the Congo, where a separate, unrelated outbreak of EVD is occurring, is also provided (2).
The purpose of this review is to provide general background information on Ebola virus disease (EVD) and specifically addresses what is known about EVD in pregnancy and the implications for practicing obstetricians and gynecologists. As the information evolves, more information will be available on Centers of Disease Control and Prevention (CDC) and World Health Organization (WHO) web sites. Limited evidence suggests that pregnant women are at increased risk for severe illness and death when infected with Ebola virus, but there is no evidence to suggest that pregnant women are more susceptible to EVD. Although it is very unlikely that obstetricians and gynecologists will diagnose or treat a patient with EVD in United States, it is important that all health care providers are prepared to respond to ensure that Ebola-virus-transmission is contained. Specifically, U.S. health care providers, including obstetricians and gynecologists, should ask patients about recent travel to affected countries in West Africa, know the signs and symptoms of EVD, and know what to do if they have a patient with compatible illness.
Background on Ebola
Ebola virus disease (EVD) is a rare but severe viral hemorrhagic fever that is caused by five different species of Ebola virus. The virus species causing the current epidemic (Zaire ebolavirus) first was identified in 1976 when there was an outbreak of viral hemorrhagic fever near the Ebola River in Zaire (now the Democratic Republic of the Congo) (3). Human disease occurs initially through direct contact with bats or their excretions or through contact with animals (e.g. great apes) that have been infected by bats (3). According to UNICEF, women are being disproportionately affected by this current Ebola outbreak (4). This is likely the result of their role as caregivers for sick children and other family members as well as their roles as health care providers and birth attendants.
Key Facts
- Ebola virus disease (EVD), formerly known as Ebola hemorrhagic fever, is a severe, often fatal illness in humans;
- The virus is transmitted to people from wild animals and spreads in the human population through human-to-human transmission;
- The average EVD case fatality rate is around 50%. Case fatality rates have varied from 25% to 90% in past outbreaks;
- The first EVD outbreaks occurred in remote villages in Central Africa, near tropical rainforests, but the most recent outbreak in west Africa has involved major urban as well as rural areas;
- Community engagement is key to successfully controlling outbreaks. Good outbreak control relies on applying a package of interventions, namely case management, surveillance and contact tracing, a good laboratory service, safe burials and social mobilization;
- Early supportive care with rehydration, symptomatic treatment improves survival. There is as yet no licensed treatment proven to neutralize the virus but a range of blood, immunological and drug therapies are under development;
- There are currently no licensed Ebola vaccines but two potential candidates are undergoing evaluation.
Transmission
It is thought that fruit bats of the Pteropodidae family are natural Ebola virus hosts. Ebola is introduced into the human population through close contact with the blood, secretions, organs or other bodily fluids of infected animals such as chimpanzees, gorillas, fruit bats, monkeys, forest antelope and porcupines found ill or dead or in the rainforest (3). Ebola then spreads through human-to-human transmission via direct contact (through broken skin or mucous membranes) with the blood, secretions, organs or other bodily fluids of infected people, and with surfaces and materials (e.g. bedding, clothing) contaminated with these fluids. Health-care workers have frequently been infected while treating patients with suspected or confirmed EVD. This has occurred through close contact with patients when infection control precautions are not strictly practiced. Burial ceremonies in which mourners have direct contact with the body of the deceased person can also play a role in the transmission of Ebola. People remain infectious as long as their blood and body fluids, including semen and breast milk, contain the virus. Men who have recovered from the disease can still transmit the virus through their semen for up to 7 weeks after recovery from illness.
Symptoms of Ebola Virus Disease (EVD)
The incubation period, that is, the time interval from infection with the virus to onset of symptoms is 2 to 21 days. Humans are not infectious until they develop symptoms. First symptoms are the sudden onset of fever, fatigue, muscle pain, headache and sore throat. This is followed by vomiting, diarrhea, rash, symptoms of impaired kidney and liver function, and in some cases, both internal and external bleeding (e.g. oozing from the gums, blood in the stools). Ebola viruses have tropism for multiple tissues, and multi-organ infection can occur (4). Ebola virus infection elicits cytokine dysregulation resulting in a robust host inflammatory response and patients may progress to critical illness with multi-organ failure and septic shock (5). Other complications can include cerebral edema, seizures, coma, coagulopathy, and hemorrhagic manifestations. Although past outbreaks have been associated with almost 90% mortality, the case-fatality proportion in this outbreak is approximately 55-75% (6).
Laboratory findings include low white blood cell and platelet counts and elevated liver enzymes. Various tests are available for accurate diagnosis (discussed below).
Diagnosis
It can be difficult to distinguish EVD from other infectious diseases such as malaria, typhoid fever and meningitis. Confirmation that symptoms are caused by Ebola virus infection are made using the following investigations:
- Antibody-capture enzyme-linked immunosorbent assay (ELISA);
- Antigen-capture detection tests;
- Serum neutralization test;
- Reverse transcriptase polymerase chain reaction (RT-PCR) assay;
- Electron microscopy;
- Virus isolation by cell culture.
Samples from patients are an extreme biohazard risk; laboratory testing on non-inactivated samples should be conducted under maximum biological containment conditions (7).
| Timeline of Infection | Diagnostic Tests Available |
Within a few days after symptoms begin |
|
|
Later in disease course or after recovery |
IgM and IgG antibodies; |
|
Retrospectively in deceased patients |
|
Treatment and Vaccines
Supportive care-rehydration with oral- or intravenous-fluids and treatment of specific symptoms, improves survival. There is as yet no proven treatment available for EVD (8). However, a range of potential treatments including blood products, immune therapies and drug therapies are currently being evaluated. No licensed vaccines are available yet, but two potential vaccines are undergoing human safety testing (8).
Clinical management consists of supportive care, particularly fluid and electrolyte management, correction of coagulopathy, treatment of secondary infections, and management of other complications. A critical element of clinical management is prompt isolation and implementation of recommended infection-control measures (standard, contact, droplet precautions) using appropriate personal protective equipment for persons who are under investigation and patients with confirmed EVD (8). Several investigational therapeutics are in development but either lack human data or have very limited availability. There is no approved Ebola vaccine, but Ebola vaccines are in development, and phase I trial of some vaccines are planned for initiation soon (9). The most effective way to stop the current outbreak is early identification of persons with possible Ebola virus infection, followed by isolation and diagnostic testing, combined with tracing contacts to stop the chain of transmission. Individuals with possible Ebola exposure should be monitored for 21 days, with prompt isolation and testing for those who become symptomatic (9).
Prevention and Control
Good outbreak control relies on applying a package of interventions, namely case management, surveillance and contact tracing, a good laboratory service, safe burials and social mobilization. Community engagement is key to successfully controlling outbreaks. Raising awareness of risk factors for Ebola infection and protective measures that individuals can take is an effective way to reduce human transmission. Risk reduction messaging should focus on several factors:
- Reducing the risk of wildlife-to-human transmission from contact with infected fruit bats or monkeys/apes and the consumption of their raw meat. Animals should be handled with gloves and other appropriate protective clothing. Animal products (blood and meat) should be thoroughly cooked before consumption;
- Reducing the risk of human-to-human transmission from direct or close contact with people with Ebola symptoms, particularly with their bodily fluids. Gloves and appropriate personal protective equipment should be worn when taking care of ill patients at home. Regular hand washing is required after visiting patients in hospital, as well as after taking care of patients at home;
- Outbreak containment measures including prompt and safe burial of the dead, identifying people who may have been in contact with someone infected with Ebola, monitoring the health of contacts for 21 days, the importance of separating the healthy from the sick to prevent further spread, the importance of good hygiene and maintaining a clean environment;
- Controlling infection in health-care settings: Health-care workers should always take standard precautions when caring for patients, regardless of their presumed diagnosis. These include basic hand hygiene, respiratory hygiene, use of personal protective equipment (to block splashes or other contact with infected materials), safe injection practices and safe burial practices.
Health-care workers caring for patients with suspected or confirmed Ebola virus should apply extra infection control measures to prevent contact with the patient’s blood and body fluids and contaminated surfaces or materials such as clothing and bedding. When in close contact (within 1 meter) of patients with EBV, health-care workers should wear face protection (a face shield or a medical mask and goggles), a clean, non-sterile long-sleeved gown, and gloves (sterile gloves for some procedures). Laboratory workers are also at risk. Samples taken from humans and animals for investigation of Ebola infection should be handled by trained staff and processed in suitably equipped laboratories.
WHEC General Travel Advice:
- Travelers should avoid all contact with infected patients;
- Health workers traveling to affected areas should strictly follow WHO-recommended infection control guidance;
- Anyone who has stayed in areas where cases were recently reported should be aware of the symptoms of infection and seek medical attention at the first sign of illness;
- Clinicians caring for travelers returning from affected areas with compatible symptoms are advised to consider the possibility of EVD.
For additional travel advice, please read the Travel and transport risk assessment: Recommendations for public health authorities and transport sector at http://who.int/ith/updates/20140421/en/
Ebola Virus Disease (EVD) in Pregnancy
Much of what we know about Ebola in pregnancy comes from previous outbreaks of EVD in Africa. However, in the resource-limited settings where EVD outbreaks generally occur, pregnancy information is not usually systematically collected. Limited evidence suggests that pregnant women are at increased risk for serve illness and death when infected with Ebola virus, but there is no evidence to suggest that pregnant women are more susceptible to Ebola virus infection (10). In addition, pregnant women with EVD seem to be at an increased risk for spontaneous abortion and pregnancy-related hemorrhage (10). Neonates born to mothers with EVD have not survived, and the causes of these deaths are uncertain (11).
In 1976, there were 318 cases of an acute viral hemorrhagic fever in the Yambuku area of Zaire (now the Democratic Republic of the Congo). The virus later was identified as Ebola virus, and the outbreak was linked to receipt of injections with contaminated needles in a hospital setting. Although a disproportionate number of pregnant women were affected (46% of 177 Ebola-infected were pregnant), this was largely attributed to the receipt of vitamin injections that were given as part of routine prenatal care. During this outbreak, overall mortality (88%) as well as mortality among pregnant women (89%) were high. Among the 82 pregnant, 19 (23%) had spontaneous abortions, including first-trimester and second-trimester losses. Among 11 neonates born to mothers with EVD, all died within 19 days of life; 7 of the 11 neonates had fever. It is not known whether these neonatal deaths were due to perinatally acquired infection with Ebola virus or to other causes, such as endemic infections (e.g. malaria, typhoid) or malnourishment (12).
During an outbreak in 1996 in Kikwit, Democratic Republic of the Congo, 105 women were identified with EVD; 15 (14%) were or had been pregnant during their illness (10). All 15 of these women developed vaginal and uterine bleeding, and 14 died within 10 days of illness onset; one woman survived despite hemorrhage-induced hypovolemic shock after fetal loss. Among hospitalized patients, 14 of 15 (93%) pregnant women died compared with 28 of 40 (70%) non-pregnant women. In terms of fetal outcomes, among the 10 women who presented in the first or second trimester of pregnancy, all experienced spontaneous abortion. Among the 5 third-trimester pregnancies, all resulted in fetal or neonatal loss. One live-born neonate died on the third day of life with fever; the mother of this neonate died from postpartum hemorrhage. Pregnant women more likely than the overall patient population with EVD to have hemorrhagic complications, specifically vaginal and uterine bleeding associated with abortion or delivery (10).
Among 15 cases of EVD identified in Guinea early in the current outbreak, a 16-year-old patient experienced spontaneous abortion and survived (13). No other data on pregnancy outcomes are available from current outbreak.
Maternal and Child Health Issues in Africa
Because this devastating outbreak is occurring largely in resource-constrained settings, it is likely that already overburdened health care services will be weakened further. This may affect access to critical emergency obstetric services such as cesarean delivery. In addition, without enough adequately trained staff and hospitals equipped to provide personal protective equipment and to implement infection-control procedures, hospitals, and obstetric wards in particular, may serve as “amplification points” for Ebola virus transmission to health care personnel and other patients (14). Thus, women requiring emergency pregnancy-related care may be reluctant to access services. Furthermore, because prior Ebola outbreaks have been associated with contaminated needles, women may be reluctant to receive injections. Progestin injectables are a common form of contraception in affected areas, and uptake may be reduced, resulting in increased rates of unintended pregnancy (15). Lastly, fear of contaminated needles could result in decreased vaccination rates among pregnant women and their children.
Another critical issue is how mothers with suspected or confirmed EVD will safely feed their newborns and infants in these settings. In the vast majority of situations, particularly in resource-limited settings, breastfeeding is the optimal method of newborn and infant feeding. During Ebola outbreak, decisions about how mothers should feed their newborns and infants are particularly complicated. Although Ebola virus has been detected in breast milk, it is unknown whether Ebola virus can be transmitted from mothers to infants through breastfeeding, but given what is known about Ebola virus transmission and evidence from other viral infections, it seems likely that ill mothers would be at high risk for transmitting the virus to their newborns and infants through breast milk and close contact, including the act of suckling (16). Virtually nothing is known about the clearance of Ebola virus from breast milk in convalescing women. However, in many of these settings, there may not be a safe alternative to breastfeeding. In resource-limited settings, non-breastfed infants may be at increased risk of death from starvation and other infectious diseases such as diarrheal and respiratory diseases (17). In addition, there may be concern about whether an infant exposed to a mother with EVD poses a contact risk to other caregivers.
Pregnant Woman with Fever Presenting to Labor and Delivery Services
Among the approximately 4 million women who give birth in the United States each year, fewer than 8,000 (less than 0.2%) are reported as non-residents in vital statistics data (18). Thus, the number of pregnant women in the United States who are residents of the Ebola-affected countries is likely to be small. Despite this, obstetric providers who care for foreign-born women or women with a recent travel history should become familiar with Ebola signs and symptoms and transmission. Women with fever or other signs and symptoms of EVD should be asked about recent travel history (within 21 days) to affected areas – Liberia, Sierra Leone, Guinea, and Nigeria. Clinical signs and symptoms of EVD include fever of 38.6°C or higher and additional symptoms such as severe headache, muscle pain, vomiting, diarrhea, abdominal pain, or unexplained hemorrhage. The differential diagnosis also should include other, much more common causes of fever in EVD – endemic areas such malaria and typhoid as well as obstetric causes (e.g. chorioamnionitis) (19). Until a diagnosis of EVD can be ruled out, the patient should be isolated and infection-control precautions implemented.
In the very unlikely event that a pregnant woman in the United States is diagnosed with EVD, the clinical guidance would be the same as for non-pregnant adults, with an emphasis on monitoring for and early treatment of hemorrhagic complications. Although pregnant women may be more at risk for severe complications from EVD, the same general principles for care would apply whether or not the patient is pregnant. Standard treatment for EVD in the United States is supportive therapy to maintain plasma volume and blood pressure, electrolyte balance, and oxygenation. Correction of coagulopathy, including early and prompt treatment with blood products, and treatment of obstetric hemorrhage after delivery or fetal loss will be especially important. In addition, secondary infections and other complications should be managed appropriately (8). Spontaneous abortion appears to be common among women with EVD, and high neonatal mortality rates among Ebola virus-infected women have been reported (2),(10). Although there is little information available to ascribe the cause of death definitively as EVD for these neonates, it seems prudent to observe all of the infection-control precautions used for other probable and confirmed cases when caring for the neonates of infected women.
For all healthcare providers, infection-control procedures are recommended, including standard, contact, and droplet precautions. Health care workers involved in aerosol-generating procedures (e.g. intubation, airway suctioning) should wear respiratory-protective devices, and these procedures should be performed in an Airborne Infection Isolation Room when feasible. Given that many procedures performed as part of routine obstetric care involve potential body fluid exposure, additional personal protective equipment (e.g. double gloves, shoe covers, and leg coverings) is recommended, along with strict adherence to infection-control protocols.
Summary
Most hospitals in the United States have private rooms and adequate supplies and staff trained to adhere to recommended infection-control procedures. With strict adherence to infection control, it is highly unlikely that Ebola would pose any substantial risk of spread in the United States. However, given the increased risk of body fluid exposure, obstetric units caring for patients with EVD should employ additional personal protective equipment, such as shoe covers, double gloves and leg covers. Many NGOs in collaboration with WHO working in Africa are providing logistical and scientific support to field staff and key partners, staff members are developing and disseminating guidance on a variety of Ebola issues, including how to prevent, diagnose, and treat EVD. Recommendations regarding travel to and from affected areas; how to protect health care workers; how to trace contacts of persons with EVD; and how lactating women in affected areas should feed and care for their infants are also available in this review.
West Africa is currently in the midst of the largest Ebola outbreak in history. Although there have been no Ebola virus disease cases identified in the United States, two U.S. health care workers with EVD were medically evacuated from Liberia to the United States in early August 2014. The Centers for Disease Control and Prevention has been working closely with other U.S. government agencies and international and NGO partners for several months to respond to this global crisis. Limited evidence suggests that pregnant women are at increased risk for severe illness and death when infected with Ebola virus, but there is no evidence to suggest that pregnant women are more susceptible to EVD. In addition, pregnant women with EVD appear to be at an increased risk for spontaneous abortion and pregnancy-associated hemorrhage. Neonates born to mothers with EVD have not survived. Although it is very unlikely that obstetrician and gynecologists in the United States will diagnose or treat a patient with Ebola virus disease, it is important that all health care providers are prepared to evaluate and care for these patients. Specifically, U.S. health care providers, including obstetricians and gynecologists, should ask patients about recent travel and should know the signs and symptoms of EVD and what to do if assessing a patient with compatible illness.
Suggested Reading
- World Health Organization
Consolidated Ebola Virus Disease Preparedness Checklist
http://www.who.int/csr/disease/ebola/evd-preparedness-checklist-en.pdf - National Institutes of Health (NIH)
Infection Prevention and Control Recommendations for Hospitalized Patient with Known or Suspected Ebola Virus Disease in U.S. Hospital
http://www.nih.gov/health/ebola.htm#/121220
References
- Centers for Disease Control and Prevention. 2014 Ebola out-break in West Africa. Available at: http://www.cdc.gov/vhf/ebola/ Accessed on 21 October 2014
- World Health Organization. The Ebola Response Roadmap is available at: http://www.who.int/csr/resources/publications/ebola/response-roadmap/en/ Accessed on 23 October 2014
- Feldmann H, Geisbert TW. Ebola hemorrhagic fever. Lancet 2011;377:849-862
- United Nations Radio. UNICEF: women most affected Ebola outbreak in W. Africa. Available at: http://www.unicef.org/emergencies/ebola/75941_76137.html Accessed on 23 October 2014
- Wong G, Kobinger GP, Qiu X. Characterization of host immune responses in Ebola virus infections. Expert Rev Clin Immunol 2014;10:781-790
- Green A. WHO and partners launch Ebola response plan. Lancet 2014;384:481
- Dixon MG, Schafer IJ. Ebola viral disease outbreak – West Africa, 2014. MMWR Morb Mortal Wkly Rep 2014;63:548-551
- Centers for Disease Control and Prevention. Questions and answers on experimental treatment and vaccines for Ebola. Available at: http://www.cdc.gov/vhf/ebola/outbreaks/guinea/qa-experimental-treatments.html Accessed on 23 October 2014
- Wong G, Qiu X, Olinger GG, Kobinger GP. Post-exposure therapy of filovirus infections. Trends Microbiol 2014;22:456-463
- Mupapa K, Mukundu W, Bwaka MA, et al. Ebola hemorrhagic fever and pregnancy. J Infect Dis 1999:179(suppl 1):S11.12
- World Health Organization. Ebola hemorrhagic fever in Zaire, 1976. Bull World Health Organ 1978;56:271-293
- Jamieson DJ, Uyeki TM, Callaghan WM, et al. What obstetricians-gynecologists should know about Ebola. Obstet Gynecol 2014 [epub ahead of print]
- Baize S, Pannetier D, Oestereich K, et al. Emergence of Zaire Ebola virus disease in Guinea – preliminary report. N Engl J Med 2014 [epub ahead of print]
- Gostin LO, Lucey D, Phelan A. The Ebola epidemic: a global health emergency. JAMA 2014 [epub ahead of print]
- Liberia Institute of Statistics and Geo-Information Services, Ministry of Health and Social Welfare, National AIDS Control Program, MEASURE DHS, ICF International. Liberia demographic and health survey 2013: preliminary report. Available at: http://www.dhsprogram.com/pubs/pdf/PR39/PR39.pdf Accessed on 22 October 2014
- Bausch DG, Towner JS, Dowell SF, et al. Assessment of the risk of Ebola virus transmission from bodily fluids and fomites. J Infect Dis 2007;196(suppl 2):S142-S147
- World Health Organization. Effect of breastfeeding on infant and child mortality due to infectious diseases in less developed countries: a pooled analysis. WHO Collaborative Study Team on the Role of Breastfeeding on the Prevention of Infant Mortality. Lancet 2000;355:451-455
- Center for Disease Control and Prevention. Vital statistics data available online. Birth data files. 2014. Available at: http://www.cdc.gov/nchs/data_access/Vitalstatsonline.htm Retrieved 22 October 2014
- Centers for Disease Control and Prevention. Ebola virus disease information for clinicians in U.S. healthcare settings. Available at: href=http://www.cdc.gov/vhf/ebola/hcp/clinician-information-us-healthcare-settings.html Retrieved 18 October 2014
Опубликован: 24 October 2014
Dedicated to Women's and Children's Well-being and Health Care Worldwide
www.womenshealthsection.com


