Vulvodynia
WHEC Practice Bulletin and Clinical Management Guidelines for healthcare providers. Educational grant provided by Women's Health and Education Center (WHEC).
Vulvovaginal disorders are increasingly recognized as a source of significant pain and discomfort and lead to a substantial decrease in quality of life for many women. The condition that we now know as vulvodynia was first described in 1889 as "excessive sensitive" or " hyperesthesia'' of the vulva by Skene, who noted that despite the absence of visible manifestation of vulvar disease, some patients experienced exquisite pain. More than a century later, this description of vulvodynia remains apt.
The pain of vulvodynia can range from minor to severe where even the touch of clothing against the skin produces an agonizing sensation. It is a chronic discomfort or pain characterized by burning, stinging, irritation, and rawness of the female genitalia. Women with vulvodynia may experience pain continuously or intermittently. Further, the pain may be either diffuse throughout the vulvar area or localized to one specific place. Vulval vestibulitis, a subset of vulvodynia, refers to pain that is experienced only when pressure is applied to the vestibule, the area immediately surrounding the vaginal opening.
The purpose of this document is to discuss signs, symptoms and management of vulvodynia. Provoked vestibulodynia, formerly referred to as vulvar vestibulitis syndrome, is suspected to be the most frequent type of vulvodynia in premenopausal women. In addition to disrupting sexual functioning, there is preliminary evidence to suggest that this pain problem can adversely affect general psychological well-being and overall quality of life. Despite its high prevalence and associated negative sequelae, there is a dearth of controlled treatment outcome studies focusing on vulvodynia. Although there are now several published studies evaluating different treatment approaches for vestibulodynia, there are only a handful of randomized trials, resulting in a hodgepodge of interventions for which there is little empirical support. Thus, current guidelines and recommendations are largely based on clinical observations and uncontrolled data rather than being anchored in findings from rigorous studies.
Incidence:
Although few data assess how prevalent vulvodynia is, an incidence of 15% has been reported. The literature describes a set of characteristics common to vulvodynia sufferers: 97% are white, 55% are nulliparous (had no pregnancy) and the mean age is 36 years (range 11-80 years). Most have experienced vulvar discomfort for years before seeking help, and the vast majority sees multiple physicians in their quest for relief. A recent population-based study suggests that 16% of women in the United States alone may experience chronic unexplained vulval pain, or vulvodynia, during their lifetime. It is characterized by a severe, burning, or sharp pain that occurs in response to pressure localized to the vestibule, with prevalence estimates ranging from 12% in the general population to 15% in general gynecological practice (1). Very little is known about the natural history of vestibulodynia and where the magnitude of placebo effects resulting from pain interventions is thought to be high. Some clinicians hold reservations about surgery and warn that it should be recommended only after failure of more conservative treatments; others claim that there are few data to justify this cautionary statement.
Terminology and Classification:
Individuals with vulvodynia are often reported to seek help from multiple clinicians in an attempt to establish a diagnosis for their condition and effective alleviation of their symptoms. Many women experience vulvar pain and discomfort that affects the quality of their lives. Vulvodynia is described by most patients as burning, stinging, irritation, or rawness. It is a condition in which pain is present although the vulva appears normal (other than erythema). The most recent terminology and classification of vulvar pain by the International Society for the Study of Vulvovaginal Disease defines vulvodynia as "vulvar discomfort, most often described as burning pain, occurring in the absence of relevant visible findings of a specific, clinically identifiable, neurologic disorder" (2). The classification of vulvodynia is based on the site of the pain, whether it is generalized or localized, and whether it is provoked, unprovoked, or mixed. Although the term vulvar dysesthesia has been used in the past, there is now consensus to use the term vulvodynia and subcategorize it as localized or generalized (3). Characterizing the Pain:
Allodynia: a painful response of normal skin to non-noxious stimulus.
Hyperalgesia: an abnormally increased pain sense.
Dysesthesia: an unpleasant, abnormal sensation produced by normal stimuli.
Patients with vulvodynia might have all three variations. It either is pure or mixed, primary or secondary, and organic or idiopathic.
Etiology:
Because the etiology of vulvodynia is unknown, it is difficult to say whether localized vulvodynia (previously referred to as vestibulitis) and generalized vulvodynia are different manifestations of the same disease process (4). In many cases of vulvodynia, the etiology remains elusive, and there is no single factor that has been satisfactorily proven as causative. The potential sources of damage are:
Unknown stimuli
Chronic skin irritation from application of steroids, podophyllin, 5-florouracil, and feminine hygiene products
Estrogen - deficient states (atrophic vulvodynia)
Neurological compression (stretch injury, transaction of the nerve, nerve infection)
Neuromal damage (tumors, cysts)
Pelvic floor descent (prolapse with stretching of the pudendal nerve through Alcock's canal)
Soft tissue injury (vaginal delivery, aggressive laser ablation of vulvar skin, retractor pressure, automobile accident, straddle injury, episiotomy pain)
Sympathetic damage (surgery)
The Diagnostic Process:
A thorough history, physical examination, and laboratory testing are all part of the initial evaluation of the patient with vulvodynia. A detailed history is the most important part of evaluation and diagnosis. In addition to the character, quality, and duration of the symptoms, the patient is asked whether she recalls an initiating factor or use of a particular medication or relationship to menstruation. Clinical profiles suggest that more than half of women with vulvodynia may suffer from additional chronic health conditions, such as repeated yeast infection, chronic fatigue syndrome, and irritable bowel syndrome.
Categorizing the level of dysparunia that patients experience often helps clinicians to track the improvement (or lack thereof) of symptoms over time. Level 1 dysparunia causes discomfort but does not prevent intercourse; level 2 sometimes prevents intercourse; and level 3 completely prevents intercourse.
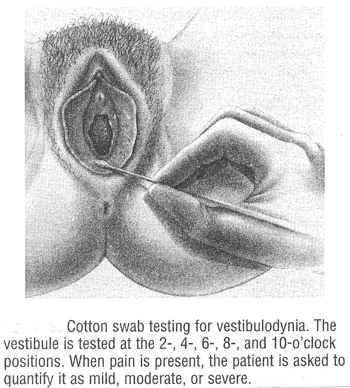
Physical Examination: A careful examination of the external genitalia is important in patients with Vulvodynia. The cotton swab test is useful for evaluation of the pain (5). The test is performed by touching the vulva lightly in specific areas with a saline-moistened cotton swab and asking the patient to rate her degree of discomfort on a scale of zero to five, with zero representing light sensation with no pain and five representing maximum stinging and burning pain. A diagram of pain locations may be helpful in assessing the pain over time.
During internal examination of the vagina, the physician should palpate the pelvic muscle, assess for pain in the areas of the coccyx, mons pubis and inner thigh, assess for prolapse and trace the course of the pudendal nerve. The vagina should be examined, and tests, including wet mount, vaginal pH, fungal culture, and Gram stain, should be performed as indicated. Fungal culture may identify but sensitivity testing usually is not required. Testing for human Papillomavirus (HPV) infection is unnecessary. Colposcopy is sometimes performed to rule out such conditions as condyloma vaginitis, vulval dystrophies and any suspicious lesions are biopsied. Vulvar biopsies are usually performed with anesthesia. Finally, a neurological examination is necessary to evaluate sphincter tone, spinal cord function, and Babinski, deep tendon and sacral reflexes.
Laboratory Testing:
Secretions from the vagina but also from the specific areas of discomfort, including the vulva and anus, are taken to rule out any infections. Blood tests are done to rule out autoimmune and endocrine disorders. If perimenopausal or premature ovarian failure is a possibility, blood should be drawn for measurement of luteal-phase serum estradiol and follicle-stimulating hormone (FSH) levels. Vulvodynia can be very difficult to diagnose and treat.
Treatment:
The treatment is focused on eliminating or relieving discomfort. If the underlying etiology is identified, treatment is focused on treating the cause if possible. Patients are advised to wear loose clothing, to refrain from exercising excessively, and to avoid activities that might produce excessive perineal irritation, including bicycling, motorcycle riding, and horseback riding.
Prolapses and scars are surgically repaired. Patients are advised to eliminate irritants; women are likely to begin to feel worse before they begin to feel better.
General care of the vulva is advised. The following vulval care measures can minimize vulvar irritations: wear 100% cotton underwear (no underwear at night); avoiding vulvar irritants (perfumes, dyes, shampoos, detergents) and douching; using mild soaps for bathing, with none applied to vulva, cleaning the vulva with water only; avoiding the use of hair dryers on the vulvar area; patting the area dry after bathing, and applying a preservative-free emollient (such as vegetable oil or plain petrolatum) topically to hold moisture in the skin and improve the barrier function; switching to 100% cotton menstrual pads (if regular pads are irritating); using adequate lubrication for intercourse; applying cool gel packs to the vulvar area; rinsing and patting dry the vulva after urination.
Different medications have been tried as treatments for vulvar pain. These include topical, oral, and intralesional medications, as well as pudendal nerve blocks. Topical anesthetic agents, such as benzocaine and lidocaine, can also be used to lessen or blunt vulvar pain, but do not change the course of or eliminate the cause of the underlying pain. Although topical steroids generally do not help patients with vulvodynia, trigger-point injections of a combination of steroid and bupivacaine have been successful for some patients with localized vulvodynia (6). Topical steroids are also sometimes helpful. Patients with vulvar vestibulitis may benefit from topical estrogen therapy applied to gland opening twice a day. Self-report of chronic yeast infections and urinary tract infections (each defined as 3 or more infections within 12 months) were the strongest predictors of vulvodynia in both univariate and multivariate models. Consistent with this finding, nearly 30% cases believed that their vulvodynia was caused in part by yeast infections (7).
Biofeedback and physical therapy also are used in the treatment of both localized and generalized vulvodynia. Physical therapy techniques include internal (vaginal and rectal) and external soft tissue mobilization and myofascial release; trigger-point pressure; visceral, urogenital, and joint manipulation; electrical stimulation; therapeutic exercises; active pelvic floor training; instruction in dietary revisions; therapeutic ultrasonography; and home vaginal dilatation.
When the pain of vulvodynia has been present for a prolonged period and a precise etiology cannot be identified, patients may be started on oral antineuralgia antidepressants. It is important to explain to the patient that antidepressants are used for their suppressive effect on cutaneous nerve endings, and not for their psychotropic effect; otherwise, a patient might assume that she is covertly being treated for a depressive disorder. The tricyclic antidepressant amitriptyline has been found to be effective in this application. The patient should be started with low dose of 10 mg daily, increasing in 10 mg increments every 1 to 2 weeks, if necessary, to a maximum daily dosage of 60 mg. Patients should continue at the highest dose they can tolerate for a minimum of 2 to 6 months. When relief is obtained, the dose can be tapered to the minimum dose required to control the symptoms.
Surgical management: Sometimes as a therapy of last resort, surgical excision of the major and minor vestibular glands can be effective in relieving this type of vulvar pain (8). Vestibulectomy has been helpful for many patients with localized pain that has not responded to previous treatments. Patients should be evaluated for vaginismus and if present, treated before a vestibulectomy is performed. Moreover, poorer outcome of these treatments can be predicted by increased pre-treatment pain and eroto-phobia -- the tendency to respond with negative affect to sexual cues. For generalized vulvar burning unresponsive to previous behavioral and medical treatments, referral to pain specialist may be helpful (9). Above all, the acknowledgement that the pain is real - even when its precise cause cannot be found - is essential.
Summary:
Vulvodynia is a cryptic condition that, to a great degree, continues to elude medical understanding. In recent years, however, progress has been made in identifying therapies that can relieve the agony associated with this condition. Pain and discomfort can be devastating to a women's quality of life (10). Although the cause of vulvodynia often remains elusive, it is now clear that the condition is not psychogenic, but rather pathophysiologic in origin. Vulvodynia is a complex disorder that can be difficult to treat. It is described by most patients as burning, stinging, irritation, or rawness. Many treatment options have been used, including vulvar care measures, medication, biofeedback training, physical therapy, dietary modifications, sexual counseling, and surgery. A cotton swab test is used to distinguish generalized disease from localized disease. No one treatment is effective for all patients. A number of measures can be taken to prevent irritation, and several medications can be used to treat the condition. Rapid resolution is unusual, even with appropriate therapy. Expectations for improvement need to be realistically addressed with the patient. Emotional and psychologic support is important for many patients, and sex therapy and counseling may be beneficial.
References:
- Harlow BL, Stewart EG. A population-based assessment of chronic unexplained vulvar pain: have we underestimated the prevalence of vulvodynia? J Am Med Womens Assoc 2003;58:82-88
- Moyal-Barraco M, Lynch PJ. 2003 ISSVD terminology and classification of vulvodynia: a historical perspective. J Reprod Med 2004;49:772-777
- ACOG Committee Opinion. Vulvodynia. Number 345, October 2006
- Haefner HK, Collins ME, Davis GD et al. The vulvodynia guide line. J Low Genit Tract Dis 2005;9:40-51
- Haefner HK. Critique of new gynecologic surgical procedures: surgery for vulvar vestibulitis. Clin Obtet Gynecol 2000;43:689-700
- Segal D, Tifheret H, Lazer S. Submucous infiltration of betamethasone and lidocaine in the treatment of vulvar vestibulitis. Eur J Obstet Gynecol Reprod Biol 2003;107:105-106
- Bornstein J, Livnat G, Stolar Z et al. Pure versus complicated vulvar vestibulitis: a randomized trial of fluconazole treatment. Gynecol Obstet Invest 2000;50:194-197
- Goldstein AT, Klingman D, Christopher K et al. Surgical treatment of vulvar vestibulitis syndrome: outcome assessment derived from a postoperative questionnaire. J Sex Med 2006;3:923-931
- Bergeron S, Khalife S, Glazer HI et al. Surgical and behavioral treatments for vestibulodynia. Obstet Gynecol 2008;111:159-166
- Arnold LD, Bachmann GA, Rosen R et al. Vulvodynia: characteristics and associations with comorbidities and quality of life. Obstet Gynecol 2006;107:617-624
Published: 23 September 2009
Dedicated to Women's and Children's Well-being and Health Care Worldwide
www.womenshealthsection.com


